Whiplash Nerve Injury: EP Wellness and Functional Medicine Clinic
Neck injuries and whiplash symptoms can be minor and go away within a few days. However, whiplash symptoms can manifest days later and become varied and chronic, ranging from severe pain to cognitive problems. These are collectively called whiplash-associated disorders because of the varied complexity of the symptoms. A common condition is a whiplash nerve injury. These injuries can be severe and require chiropractic treatment.
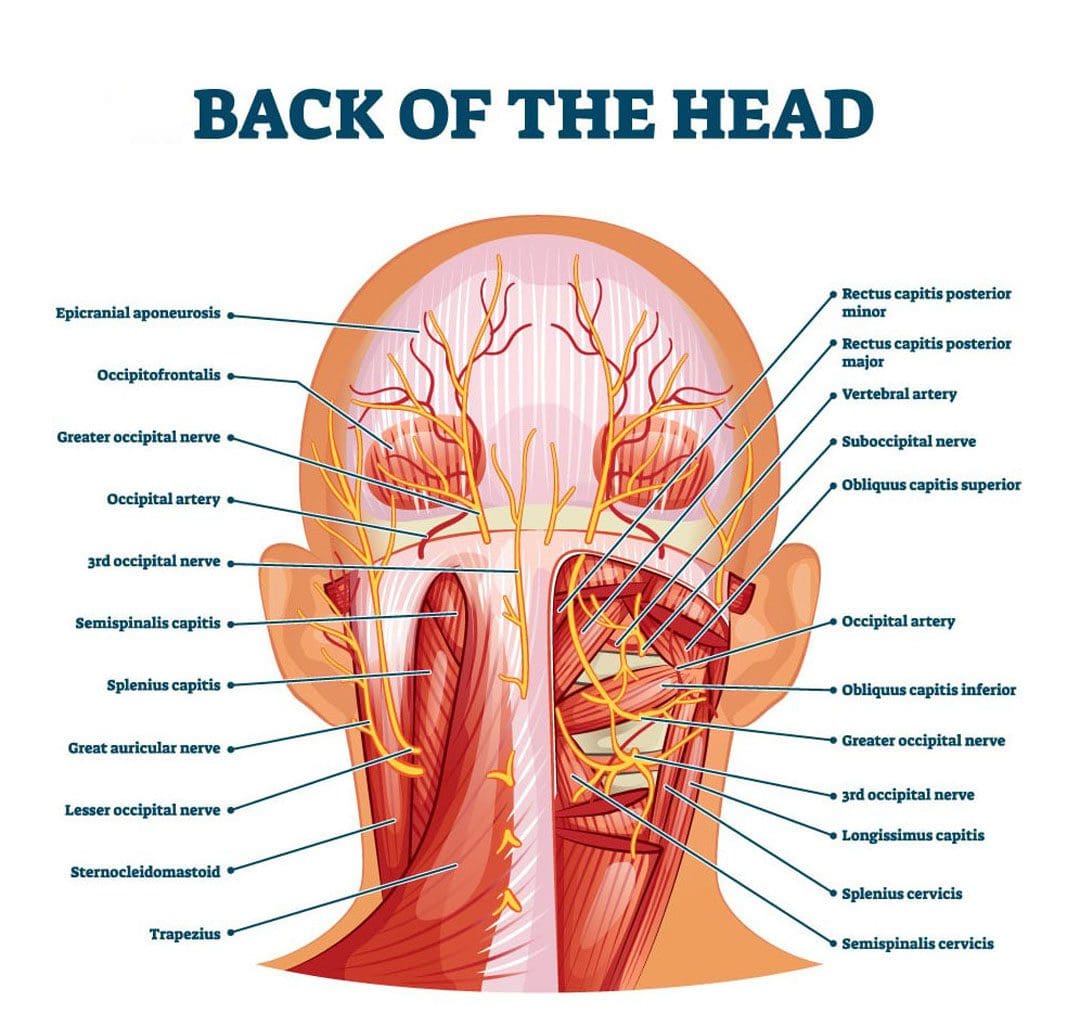 Whiplash Nerve Injury
Whiplash Nerve Injury
Surrounding muscles, tissues, bones, or tendons can cause a whiplash nerve injury. The neck’s spinal nerve roots become compressed or inflamed, leading to cervical radiculopathy symptoms of tingling, weakness, and numbness that can radiate down the shoulder, arm, hand, and fingers. Typically, cervical radiculopathy is only felt on one side of the body, but in rare cases, it can be felt on both sides if more than one nerve root is affected.
Neurological Cervical Radiculopathy
- Neurological problems can become severe and can reduce the ability to perform many routine tasks, such as gripping or lifting objects, writing, typing, or getting dressed.
Cervical radiculopathy involves one or more of the following neurological deficiencies.
- Sensory – Feelings of numbness or reduced sensation. There can also be tingling and electrical sensations.
- Motor – Weakness or reduced coordination in one or more muscles.
- Reflex – Changes in the body’s automatic reflex responses. An example is a diminished ability or reduced hammer reflex exam.
Symptoms
Because every case is different, symptoms vary depending on the location and severity. Symptoms can flare up with certain activities, like looking down at a phone. The symptoms then go away when the neck is upright. For others, symptoms can become chronic and do not resolve when the neck is resting and supported. Common symptoms include:
Fatigue
- Decreased energy levels could be related to sleep problems, depression, stress, pain, concussion, or nerve damage.
Memory and/or concentration problems
- Cognitive symptoms could involve difficulty with memory or thinking.
- Symptoms can start shortly after the injury or not appear until hours or days later.
- Cognitive problems could be from a brain injury or related to various types of stress.
Headaches
- This could be neck muscles tightening or a nerve or joint becoming compressed or irritated.
Dizziness
- Dizziness could be from neck instability, a concussion/mild traumatic brain injury, and nerve damage.
Vision problems
- Blurry vision or other visual deficits could result from any number of causes, including concussion or nerve damage.
- Vision problems could also contribute to dizziness.
Ringing in the ears
- Also called tinnitus, this can be ringing or buzzing in one or both ears and can range from intermittent and minor to constant and severe.
- Whiplash complications such as injury to the brain region that controls hearing, nerve or vascular damage, jaw injury, or stress can lead to tinnitus.
Chiropractic Care
The appropriate chiropractic treatment is unique to each whiplash nerve injury and is directed at the primary dysfunctions detected during the initial examination. A personalized treatment plan addresses factors in an individual’s work, home, and recreational activities. Treatment includes:
- Massage manual and percussive for nerve and muscle relaxation
- Decompression therapy
- Nerve release techniques
- Targeted stretches and exercises
- Ergonomics
- Health and nutritional recommendations
El Paso’s Chiropractic Team
References
Goldsmith R, Wright C, Bell S, Rushton A. Cold hyperalgesia as a prognostic factor in whiplash-associated disorders: A systematic review. Man Ther. 2012; 17: 402-10.
McAnany SJ, Rhee JM, Baird EO, et al. Observed patterns of cervical radiculopathy: how often do they differ from a standard “Netter diagram” distribution? Spine J. 2018. pii: S1529-9430(18)31090-8.
Murphy DR. History and physical examination. In: Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 2000:387-419.
Shaw, Lynn, et al. “A systematic review of chiropractic management of adults with Whiplash-Associated Disorders: recommendations for advancing evidence-based practice and research.” Work (Reading, Mass.) vol. 35,3 (2010): 369-94. doi:10.3233/WOR-2010-0996
Travell JG, Simons DG. Myofascial Pain and Dysfunction: The Trigger Point Manual. Vol. 1, 2nd ed. Baltimore, MD: Williams and Wilkens, 1999.
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



Comments are closed.