SoftWave Therapy, Chiropractic Care & Orthobiologics in Practice
Table of Contents
SoftWave Therapy, Chiropractic Care & Orthobiologics
Abstract
In this educational post, I describe how true shockwave therapy—specifically electrohydraulic SoftWave technology—stimulates tissue repair, reduces pain, and accelerates functional recovery. I explain the physics behind shockwaves, why device type matters, and how this modality integrates with chiropractic care, manual therapies, targeted exercise, and orthobiologic interventions such as platelet-rich plasma (PRP). We review clinical observations from my practice on plantar fasciitis, adductor strains, and chronic tendinopathies, and present current research on angiogenesis, neuroinflammation, mechanotransduction, and bone marrow edema. Real-world performance applications, training considerations for clinical teams, and practical protocols that improve patient comfort and adherence.
Introduction: SoftWave Into My Clinical World
A patient faced a problem: stubborn, bilateral plantar fasciitis. Working long hours on their feet, they were told that their best option was a series of cortisone injections. They declined, uncertain about masking pain without restoring tissue integrity. A colleague urged them to try a session with a SoftWave device—a true electrohydraulic shockwave delivered through a water-coupled, moldable applicator.
Their experience was telling. The day of treatment, their feet felt lighter, though the pain crept back within a few days. They did no stretching or adjunct care, yet two months later, they realized the pain had quietly receded—and it stayed away for years. That outcome changed how I view mechanobiology, regenerative signaling, and the connection between passive care and durable recovery. It also led me to bring SoftWave into my integrative chiropractic practice, where I combine it with precise manual therapies, corrective loading, and, when indicated, orthobiologics.
What follows is a clear map of what true shockwave therapy is, how it works in the body, how to distinguish it from other devices, and where it fits within a comprehensive, patient-centered plan.
Understanding Shockwave Therapy: Physics, Physiology, and Why Device Type Matters
Key point: Not all “shockwaves” are the same.
- True shockwave vs pressure wave
- Electrohydraulic vs electromagnetic vs piezoelectric generation
- Tissue-level effects: angiogenesis, mechanotransduction, nociceptive modulation, and bone remodeling
What a Shockwave Is
A true shockwave is a high-pressure, high-velocity acoustic impulse that travels faster than the speed of sound in tissue, producing a steep pressure gradient with a rapid rise time. In electrohydraulic systems, that wave is created by a spark discharge between two submerged electrodes inside a water-filled applicator. The spark forms a rapidly expanding plasma bubble; the leading edge of that bubble is a true shockwave, already at therapeutic speed and waveform as it exits the applicator. Because the wave is generated within the applicator, the therapeutic energy is consistent and can reach tissues to depths of about 12 cm, depending on the settings and coupling.
Why This Matters Physiologically
When a true shockwave reaches cell membranes, it induces transient mechanical shear and compression, momentarily increasing membrane permeability. This mechanotransduction initiates a series of signaling cascades:
- Angiogenesis and microcirculation: Shockwave upregulates vascular endothelial growth factor and stimulates endothelial nitric oxide synthase, promoting capillary sprouting and improved perfusion in ischemic or hypoperfused tissues. Improved nutrient delivery and waste clearance support tenocyte, fibroblast, and osteoblast activity (Schaden et al., 2018; ISMST Guidelines, 2024).
- Neurogenic inflammation modulation: Repeated acoustic impulses can down-modulate substance P and calcitonin gene-related peptide in peripheral nociceptors, reducing peripheral sensitization and central wind-up over time (Notarnicola & Moretti, 2012; Wang, 2012).
- Matrix remodeling: Fibroblasts and tenocytes respond by reorganizing cytoskeletal elements, aligning collagen fibers along stress lines, and normalizing tendon stiffness, especially when paired with progressive loading programs (Wu et al., 2019).
- Osteogenic effects: In bone, shockwaves can stimulate osteoblast gene expression and local microvascular changes, supporting remodeling in bone marrow edema and delayed union scenarios (Cacchio et al., 2009; Zelle et al., 2010).
Distinguishing Radial Devices From True Shockwave
- Radial (pressure wave): Generated pneumatically or mechanically, it propagates as a lower-velocity pressure wave. It disperses energy superficially, causing microtrauma that may transiently increase blood flow. Useful for short-term analgesia in superficial tissues, but has limited depth and a different mechanism of action. Patients often report more surface tenderness with radial treatments.
- True shockwave (focused/broad focus): Delivers high-energy impulses at therapeutic velocity and waveform. Reaches deeper targets (e.g., proximal plantar fascia enthesis, common extensor tendon at the lateral epicondyle, deep adductors).
Device Generation Methods
- Electrohydraulic: Shockwave forms within the applicator; consistent wavefront and depth. The SoftWave design uses a parabolic reflector to harness both a focused primary wave and a broader secondary field, allowing a larger therapeutic zone while maintaining depth.
- Electromagnetic and piezoelectric: Generate acoustic waves that converge to form a shock front outside the applicator tip, creating a small “pre-focal” zone of sub-therapeutic sound before convergence. Effective in experienced hands, but with a narrower focal volume and shorter in-tissue therapeutic segment.
Why I Prefer Electrohydraulic With Broad Focus
In daily practice, a broader therapeutic column means I can:
- Cover the entire myofascial chain involved in a kinetic lesion rather than chasing a single tender point.
- Reduce session time while maintaining dose density.
- Use biofeedback: Patients feel a clear contrast between healthy and sensitized tissue, which helps localize pathology and increases treatment engagement.
Evidence Snapshot: Outcomes and Durability
Third-party patient-reported outcomes compiled by DataBiologics suggest:
- Radial pressure-wave treatments often yield short-term benefits with regression toward baseline by 6 months.
- Focused shockwave yields moderate pain reduction at 3 months, with partial fading by 6 months.
- Electrohydraulic broad-focus (SoftWave) demonstrates persistent improvement at 6 months, which clinically aligns with treating a higher tissue volume and addressing networked myofascial contributors. While outcomes vary by condition and protocol, this durability mirrors what I see in chronic plantar fasciitis, patellar tendinopathy, and greater trochanteric pain syndromes.
How Shockwave Feels and Why Comfort Matters
Because electrohydraulic broad-focus distributes energy over a wider field, many patients describe the sensation as a tapping or firm pulsing that intensifies over irritated tissue. Comfort enables adequate energy delivery without anesthesia, which is important: nociceptive feedback helps me titrate the dose and map dysfunctional tissue. As Mark O’Malley, MD, an orthopedic surgeon and NBA consultant, notes, comfort allows higher effective dosing without sedation and supports frequent use in elite-sport schedules.
Clinical Vignette: From Adductor Strain to Faster Return-to-Sport
In professional pickleball and basketball settings, adductor strains can sideline athletes for 6–10 weeks. With integrated care—shockwave neuromodulation and perfusion, targeted adductor loading, lumbopelvic control work, and soft-tissue release—we often see a return to sport in 3–4 weeks for Grade I–II strains when tissue integrity and strength benchmarks are met. The physiologic rationale is straightforward: improved microcirculation supports sarcomere repair; reduced nociceptive drive enables earlier, graded loading; and integrative chiropractic care restores pelvic mechanics, thereby decreasing strain on the adductor origin.
Integrative Chiropractic Care: Where Shockwave Fits
My approach is systems-based and function-focused. Shockwave is not a stand-alone miracle—it is a catalyst within a coordinated plan.
- Assessment
- Regional interdependence: Foot-ankle, knee, hip, and lumbopelvic contributors to local overload
- Load capacity vs load exposure: History, activity spikes, sleep, stress, and nutrition
- Tissue health: Tendon thickness and hypoechoic regions (if ultrasound available), palpation, and functional provocation tests
- Manual therapy and adjustments
- Joint restrictions: Restoring tibio-talar and subtalar glide, sacroiliac motion, and thoracolumbar mechanics to normalize force transmission and reduce hotspot overload
- Soft-tissue techniques: Myofascial release for fascial adhesions; neural glides for peripheral sensitization; targeted instrument-assisted work where indicated
- Shockwave sequencing
- Acute or subacute: Begin with lower energy and fewer pulses to reduce hyperalgesia; emphasize pain modulation and perfusion
- Chronic tendinopathy and fasciopathy: Use evidence-based dosing windows to stimulate neovascularization and collagen remodeling
- Corrective loading
- Isometrics: Early analgesia and tendon load tolerance (e.g., 45–60 seconds x 5, mid-range angles)
- Heavy slow resistance: 12-week progression to restore tendon stiffness and muscle capacity
- Energy-storage drills: Once pain and strength thresholds are achieved, reintroduce plyometric demand appropriate to sport
- Recovery and lifestyle
- Sleep optimization, protein sufficiency, and micronutrient support (vitamin D, magnesium, collagen/gelatin with vitamin C timed 30–60 minutes pre-loading) to augment collagen synthesis
- Footwear and orthoses: Temporary offloading when enthesis is acutely inflamed, then gradual return
Why each component matters:
- Manual adjustments improve arthrokinematics, reduce aberrant reflex inhibition, and allow efficient force coupling across joints.
- Shockwave initiates a controlled mechanobiologic stimulus that the body interprets as a call to repair—without the collateral soft-tissue trauma typical of repetitive friction methods.
- Loading provides the mechanical “direction” for new collagen to align functionally, ensuring that the biochemical gains translate into durable capacity.
Plantar Fasciitis: A Deep-Dive Into Mechanisms and Management
Physiology and pain drivers
- Microtears at the enthesis, impaired perfusion, and nociceptor sensitization along the medial calcaneal branch
- Fascial stiffness that loads the proximal band excessively during toe-off
- Often linked to limited ankle dorsiflexion, weak intrinsic foot muscles, hip abductor weakness, and altered gait
Why shockwave:
- Angiogenic signaling enhances perfusion to the relatively hypovascular proximal fascia
- Nociceptor modulation reduces morning first-step pain and allows earlier engagement in loading protocols
- Matrix remodeling supports realignment of collagen fibers under guided load
Protocol I use:
- Session cadence: Once weekly for 3–6 sessions, depending on chronicity and response
- Dose strategy: Begin conservatively, identify biofeedback hotspots, and titrate to a firm but tolerable intensity
- Integrations:
- Adjustments: Talocrural, subtalar, first ray mobility
- Soft-tissue: Plantar fascia release, posterior chain myofascial work
- Exercises: Short foot drills, heel raises with slow eccentrics, calf mobility, and progressive hopping phases when pain <2/10
- Outcome measures: Pain on first steps, 10-cm visual analog scale, Foot Function Index, single-leg stance time, hop tolerance
- Expectations: Early symptomatic relief often appears within days; structural resilience requires the full 8–12-week loading arc
Adductor Strain: Practical Return-to-Play
- Phase 1: Pain modulation and gentle isometrics (adductor squeezes, 5 x 45–60 s), shockwave to adductor longus origin and adductor mass, pelvic mechanics via chiropractic adjustments
- Phase 2: Concentric-eccentric strengthening (Copenhagen progressions), trunk anti-rotation work, stride mechanics
- Phase 3: Energy storage and release (lateral bounds, decel drills), sport-specific change of direction
- Criteria-based progression: Pain-free resisted squeeze at 0° and 45° hip flexion, side-plank holds with Copenhagen support, symmetric hop tests
- Rationale: Aligns biologic healing timelines with graded mechanotransduction; shockwave speeds the pain-modulation window, enabling earlier high-quality loading
Shockwave and Orthobiologics: Strategic Combinations
Bridging needle-phobia and enhancing biologic response
About one in four patients has significant needle anxiety. Shockwave offers a noninvasive entry point that frequently reduces pain and builds trust. For appropriate candidates, it can also complement orthobiologic strategies.
Common integration models I use:
- Same-day combination
- Sequence: Blood draw (for PRP) → shockwave → injection
- Why: Immediate analgesia from shockwave improves tolerance of the injection; improved perfusion may enhance distribution. I avoid aggressive energy settings that might increase post-injection hyperemia excessively.
- Preconditioning approach
- Sequence: Shockwave 48–72 hours before PRP or bone marrow concentrate
- Why: Pre-treatment can upregulate local cytokine signaling and microvascular readiness, potentially improving graft milieu. The short window maintains cell-signaling momentum without excessive soreness on the day of injection.
- Diagnostic and informed-consent support
- Biofeedback mapping the day before the planned injection to confirm symptomatic generators in the presence of a chaperone
- Why: Aligns patient, provider, and witness on pain localization, documents concordance, and improves shared decision-making
Clinical caveats:
- Avoid direct treatment of acute full-thickness tendon ruptures or unstable fractures.
- For post-injection timelines, I typically pause shockwave for 7–10 days after PRP unless pain management exigencies dictate otherwise, then resume with modest dosing.
Performance Medicine and Team-Based Care
As Dr. Mark O’Malley, orthopedic surgeon and consultant to multiple NBA teams, has shared, the comfort profile of SoftWave enables meaningful dosing without anesthesia. In high-stakes, congested schedules, that practicality matters. In my performance clientele, we often run:
- Weekly shockwave during acute phases, then biweekly tapering
- Concurrent spinal and pelvic adjustments to maintain kinetic chain alignment
- On-field load management: acute:chronic workload ratio tracking, GPS or accelerometry data when available
- Nutrition and sleep interventions to align tissue anabolism with training blocks
Training My Team and Scaling Care
Shockwave’s broad therapeutic zone and patient biofeedback make it feasible to train medical assistants or rehabilitation techs within scope, under clinician oversight. Practical points:
- Session length: 10–15 minutes
- Documentation: Region treated, pulses, energy settings, patient-reported sensitivity map, pre/post pain scores, functional test deltas
- Safety: Water-coupled, moldable silicone interface improves contact over contours (e.g., ankles, fingers). Avoid bony prominences with high settings; adjust based on patient tolerance.
Safety, Contraindications, and Expectations
- Common, self-limited effects: Temporary soreness, mild erythema, transient paresthesia
- Relative contraindications: Pregnancy over abdomen/pelvis, active infection or osteomyelitis in the field, coagulopathy/anticoagulation (use caution), malignancy in the treatment zone, open growth plates (case-by-case), implanted electronic devices near the field
- Set expectations: True tissue remodeling unfolds over weeks; shockwave often opens a “window” of reduced pain during which corrective loading does the long-term work
How We Measure Success
I emphasize objective and subjective outcomes:
- Pain: VAS/NPRS pre and post session, morning pain logs
- Function: PROMs such as LEFS, FAAM, VISA-A/E; timed tasks; hop and strength metrics
- Load: Session-RPE x duration; weekly workload roll-ups
- Tissue: Ultrasound, where available, for tendon thickness and echotexture trends
- Durability: 3- and 6-month follow-ups to confirm lasting change, not just transient analgesia
Real-World Access and Patient Experience
A barrier to adoption has been a lack of awareness. Many people encounter “shockwave” in the form of a radial pressure wave and assume that is the full story. My aim is to ensure patients and clinicians understand:
- What device is being used
- Why true shockwave differs in mechanism and outcomes
- How it integrates with hands-on chiropractic care and exercise to create durable change
In my clinic, we routinely see patients walk in, rate their pain at 7–8/10, and leave their first session at 3–4/10. That immediate relief builds trust, but our conversations always return to the plan: adjustments for mechanics, shockwave for biologic signaling, and progressive loading for long-term resilience.
Putting It All Together: A Sample Protocol Map
- Evaluation day
- Comprehensive biomechanical assessment
- Education on pain science and load capacity
- First shockwave session with conservative dosing; adjustments to restore regional motion; start isometrics
- Weeks 1–3
- Weekly shockwave for pain modulation and perfusion
- Manual therapy and adjustments to reinforce pattern correction
- Isometrics → slow tempo eccentrics/concentrics; short-foot and foot-ankle sequencing
- Sleep and protein goals; vitamin D optimization if low
- Weeks 4–8
- Biweekly shockwave as needed based on symptoms and milestones
- Heavy, slow resistance; begin energy storage drills
- Sport-specific progressions; footwear and surface review
- If orthobiologics indicated
- Choose a same-day or 48–72-hour preconditioning approach
- Post-injection: protect the window, reintroduce the shockwave after 7–10 days with modest settings
- Maintain the loading plan adapted to comfort and markers
A Patient-Centered Final Word
The promise of modern musculoskeletal care lies in aligning physics with physiology and behavior. True shockwave therapy provides a safe, noninvasive mechanotransductive nudge that, when paired with precise chiropractic adjustments and intelligent loading, helps tissues do what they are designed to do: heal, reorganize, and perform. From a patient’s struggle with chronic pain to a practice that blends SoftWave, integrative chiropractic care, and orthobiologics, I’ve been convinced that access and education matter. Patients should not have to “know somebody” to obtain effective tools. They deserve clear explanations, thoughtful plans, and measurable outcomes.
If you are considering this pathway, bring your questions. I am committed to transparent education, individualized protocols, and collaborative care that puts your goals first.
References
- International Society for Medical Shockwave Treatment (ISMST) Guidelines: ISMST. (2024). Clinical recommendations for extracorporeal shockwave therapy across musculoskeletal indications.
- The role of ESWT in tendon and bone healing: Schaden, W., Mittermayr, R., Haffner, N., & Smolen, D. (2018). Extracorporeal shockwave therapy in musculoskeletal disorders. Archives of Orthopaedic and Trauma Surgery, 138(5), 635–653.
- Shockwave-induced analgesia and neuropeptides: Notarnicola, A., & Moretti, B. (2012). The biological effects of extracorporeal shock wave therapy on tendon tissue. American Journal of Physical Medicine & Rehabilitation, 91(12), 1094–1102.
- Shockwave and bone marrow edema/fracture healing: Cacchio, A., et al. (2009). Extracorporeal shock-wave therapy compared with surgery for nonunion of long-bone fractures. The American Journal of Sports Medicine, 37(6), 1251–1258.
- Nonunions and ESWT systematic review: Zelle, B. A., Gollwitzer, H., Zlowodzki, M., & Bhandari, M. (2010). Extracorporeal shock wave therapy: Current evidence. Journal of Orthopaedic Trauma, 24, S66–S70.
- Tendon mechanobiology and loading synergy: Wu, F., Nerlich, M., & Docheva, D. (2019). Tendon injuries: Basic science and new repair proposals. EFORT Open Reviews, 4(12), 682–692.
- SoftWave in elite sport practice commentary: O’Malley, M. J. (Expert commentary). Hospital for Special Surgery resources on ESWT in sports medicine.
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


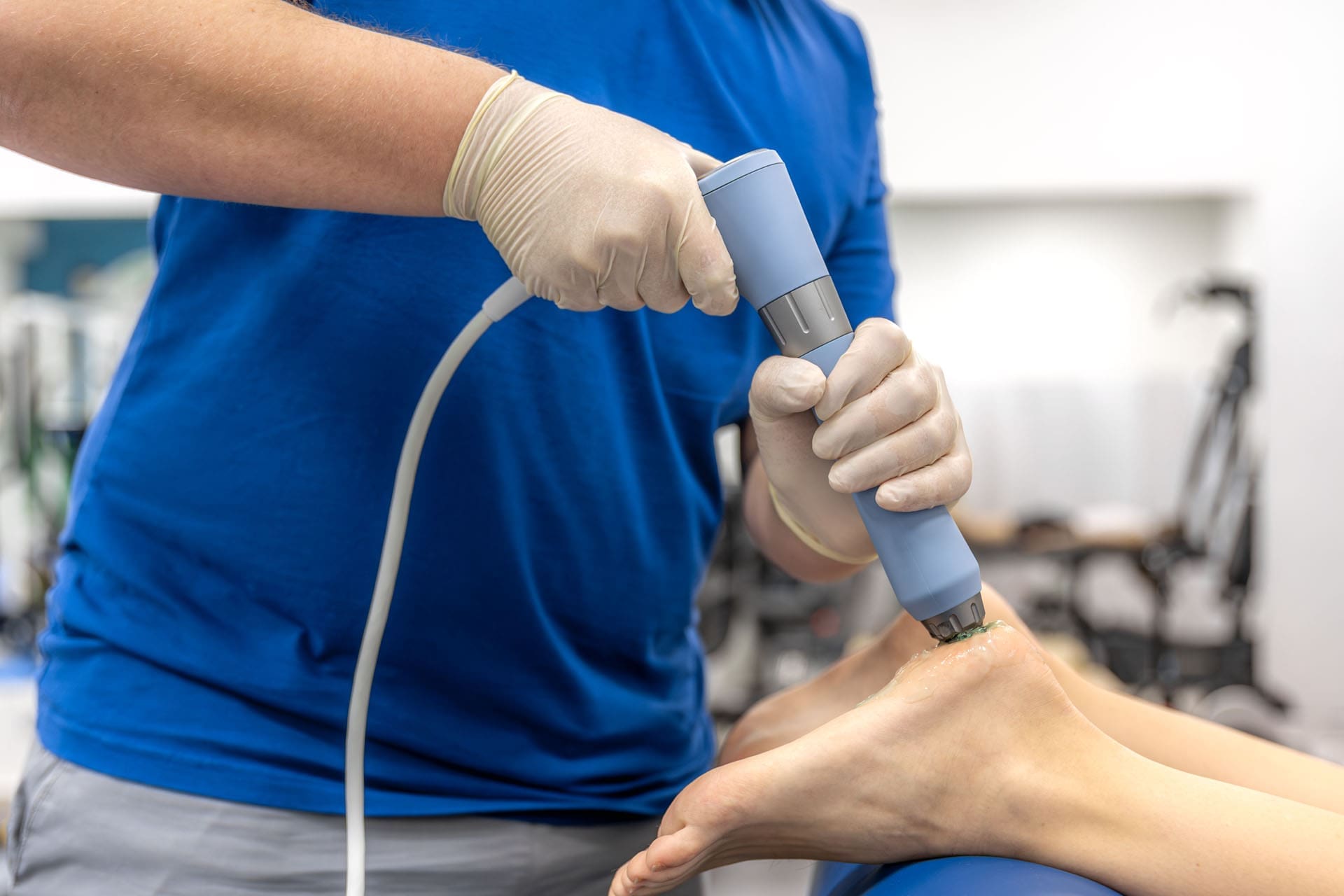
Comments are closed.