Table of Contents
Introduction
As the world is in constant motion, many people have to endure stressful situations affecting their bodies and health. The body needs hormones like cortisol to keep functioning as it affects the immune, nervous, cardiovascular, and musculoskeletal systems, to name a few. Another essential function the body needs is glucose, which requires energy to be in constant motion. Situations that cause the cortisol levels and glucose levels to rise in the body can lead to chronic issues like diabetes and chronic stress. This causes the individual to be miserable and be in a serious situation if it is not controlled right away. Today’s article examines how cortisol and glucose affect the body and the interwoven connection between stress and diabetes. Refer patients to certified, skilled providers specializing in stress management and endocrine treatments for diabetic individuals. We guide our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is critical for asking insightful questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.
How Does Cortisol Affect The Body?
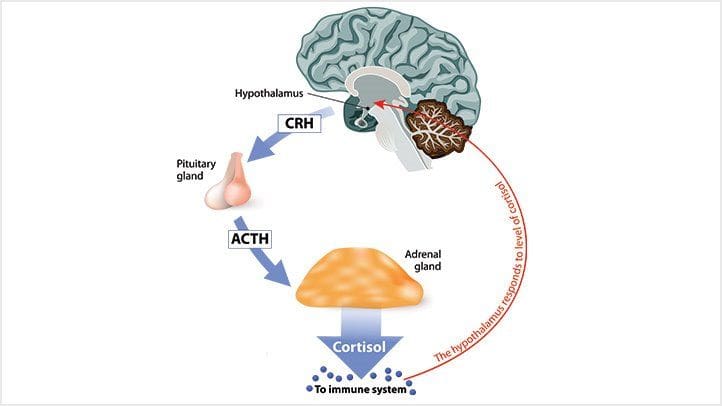
Have you been experiencing sleeping problems at night? What about frequent headaches that are a nuisance throughout the entire day? Or have you noticed excessive weight loss or weight gain around your midsection? Some of these symptoms are signs that your cortisol and glucose levels are high and can affect your body. Cortisol is a hormone produced in the endocrine system and can be beneficial or harmful to the body if it is not regularly checked. Research studies have defined cortisol as one of the prominent glucocorticoids secreted out due to the response of the body’s biochemicals, characterized by the HPA (hypothalamic‐pituitary‐adrenal) axis helps cognitive events. However, when the cortisol levels turn chronic in the body due to circumstances that cause the body to become dysfunctional, it can significantly impact a person and cause an imbalance in the HPA axis. Some of the symptoms that chronic cortisol leads to the body can include:
- Hormonal imbalances
- Insulin resistance
- Weight gain
- Increases in visceral “belly” fat
- Increased cortisol output
- Immune problems
- Allergies and Asthma
- Inflamed Joints
- Poor exercise recovery
Additional information has provided that the presence of cortisol in the body can help increase blood glucose availability to the brain. With cortisol providing organ functionality, the blood glucose provides energy for the body.
How Cortisol & Glucose Work In The Body
Cortisol helps stimulate mass glucose mobilization in the liver, allowing block protein synthesis to push amino acids into sugar for the body. This is known as fatty acid liberation biotransformed into glucose. When this happens, it helps stimulate visceral fat storage if excess glucose is not utilized, thus causing weight gain. Research studies have shown that a lack of cortisol can cause a decrease in hepatic glucose production in the body. This will cause hypoglycemia, where the body doesn’t have enough glucose in its system. Additional research shows that cortisol responds to any stressor that affects a person with low glucose levels but can also become positive after a glucose load. Managing the body’s glucose and cortisol levels can help progress the development of diabetes.
How Cortisol Is Linked With Type 2 Diabetes- Video
Have you experienced stressful situations that cause your muscles to tense up? How about feeling your blood sugar either spiking up or down? Do you feel inflammatory effects all over your body that makes them ache? Stress can cause harmful effects to the body, activating inflammation, increasing sympathetic tone, and reducing glucocorticoid responsiveness. Stress can also be linked to diabetes, as the video above shows how the stress hormone cortisol is linked with type 2 diabetes. Research studies have mentioned that cortisol can become negatively associated with the mechanics of insulin resistance, increasing the beta-cell function and increasing the insulin released in the body. This can become dangerous for many individuals that have pre-existing diabetes and have been dealing with stress constantly.
The Interwoven Connection Between Stress & Diabetes
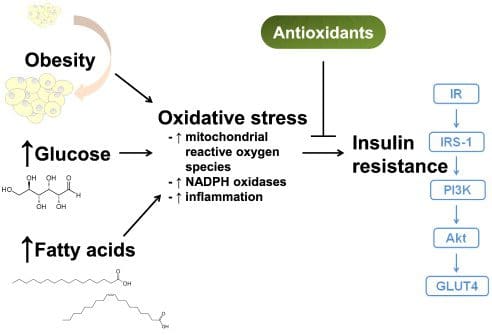
The interwoven connection between stress and diabetes is shown as research studies have found that the pathophysiology of anxiety and diabetes has increased insulin resistance risk for the body. When a person is dealing with chronic stress, it can cause them to have many issues like:
- Cold intolerance
- Diminished cognition and mood
- Food sensitivities
- Low energy throughout the day
When this happens, the body is at a high risk of developing insulin resistance and type 2 diabetes. Research studies have mentioned that type 2 diabetes is characterized by insulin resistance and beta-cell dysfunction. The glucocorticoid in the body can become excessive to affect the cells, causing dysfunctionality. Additional research studies have shown that any perceived stress can become a vital risk factor that not only affects the body, like hypertension, BMI (body mass index), or diet quality but can cause a rise in type 2 diabetes. When individuals find ways to lower their chronic stress, it can help manage their glucose levels from reaching critical levels.
Conclusion
The body’s chronic stress can cause insulin resistance and cause diabetes to become pre-existing. The body needs cortisol and glucose to keep functioning and have the energy to move. When people start to suffer from chronic stress and diabetes, it can become challenging to manage; however, making minor changes to the body like finding ways to lower stress, eating healthy foods, and monitoring glucose levels can help the body reset the glucose and cortisol levels to normal. Doing this can relieve many individuals who want to continue their health journey being stress-free.
References
Adam, Tanja C, et al. “Cortisol Is Negatively Associated with Insulin Sensitivity in Overweight Latino Youth.” The Journal of Clinical Endocrinology and Metabolism, The Endocrine Society, Oct. 2010, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3050109/.
De Feo, P, et al. “Contribution of Cortisol to Glucose Counterregulation in Humans.” The American Journal of Physiology, U.S. National Library of Medicine, July 1989, https://pubmed.ncbi.nlm.nih.gov/2665516/.
Hucklebridge, F H, et al. “The Awakening Cortisol Response and Blood Glucose Levels.” Life Sciences, U.S. National Library of Medicine, 1999, https://pubmed.ncbi.nlm.nih.gov/10201642/.
Joseph, Joshua J, and Sherita H Golden. “Cortisol Dysregulation: The Bidirectional Link between Stress, Depression, and Type 2 Diabetes Mellitus.” Annals of the New York Academy of Sciences, U.S. National Library of Medicine, Mar. 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5334212/.
Kamba, Aya, et al. “Association between Higher Serum Cortisol Levels and Decreased Insulin Secretion in a General Population.” PloS One, Public Library of Science, 18 Nov. 2016, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5115704/.
Lee, Do Yup, et al. “Technical and Clinical Aspects of Cortisol as a Biochemical Marker of Chronic Stress.” BMB Reports, Korean Society for Biochemistry and Molecular Biology, Apr. 2015, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4436856/.
Thau, Lauren, et al. “Physiology, Cortisol.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 6 Sept. 2021, https://www.ncbi.nlm.nih.gov/books/NBK538239.
Disclaimer
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



Comments are closed.