Table of Contents
Introduction
The muscles, tissues, and ligaments help stabilize the joints and structure of the spine so that the body can function. These muscles are layered and interwoven in the spine and joints that help facilitate movement. When the body suffers from injuries or traumatic events, the muscles, tissues, and ligaments become affected, causing muscle pain and discomfort. This causes the muscles to be tender to the touch and sensitive. This is known as myofascial pain syndrome. Today’s article looks at myofascial pain syndrome, how it is linked with central sensitization, and ways to manage myofascial pain syndrome. We refer patients to certified providers specializing in musculoskeletal treatments to help many individuals with myofascial pain syndrome associated with central sensitization. We also guide our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is the solution to asking our providers insightful questions. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
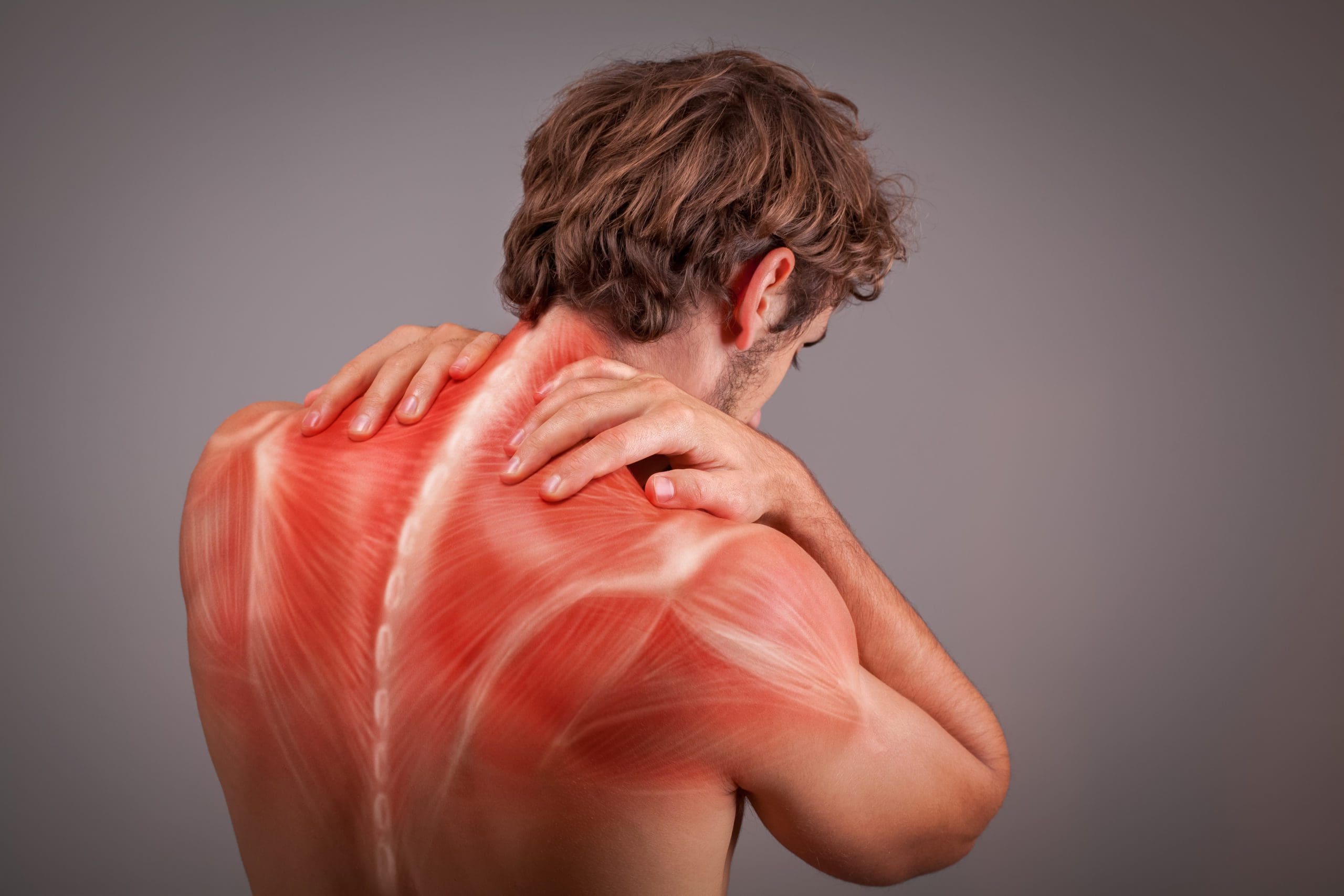
What Is Myofascial Pain Syndrome?
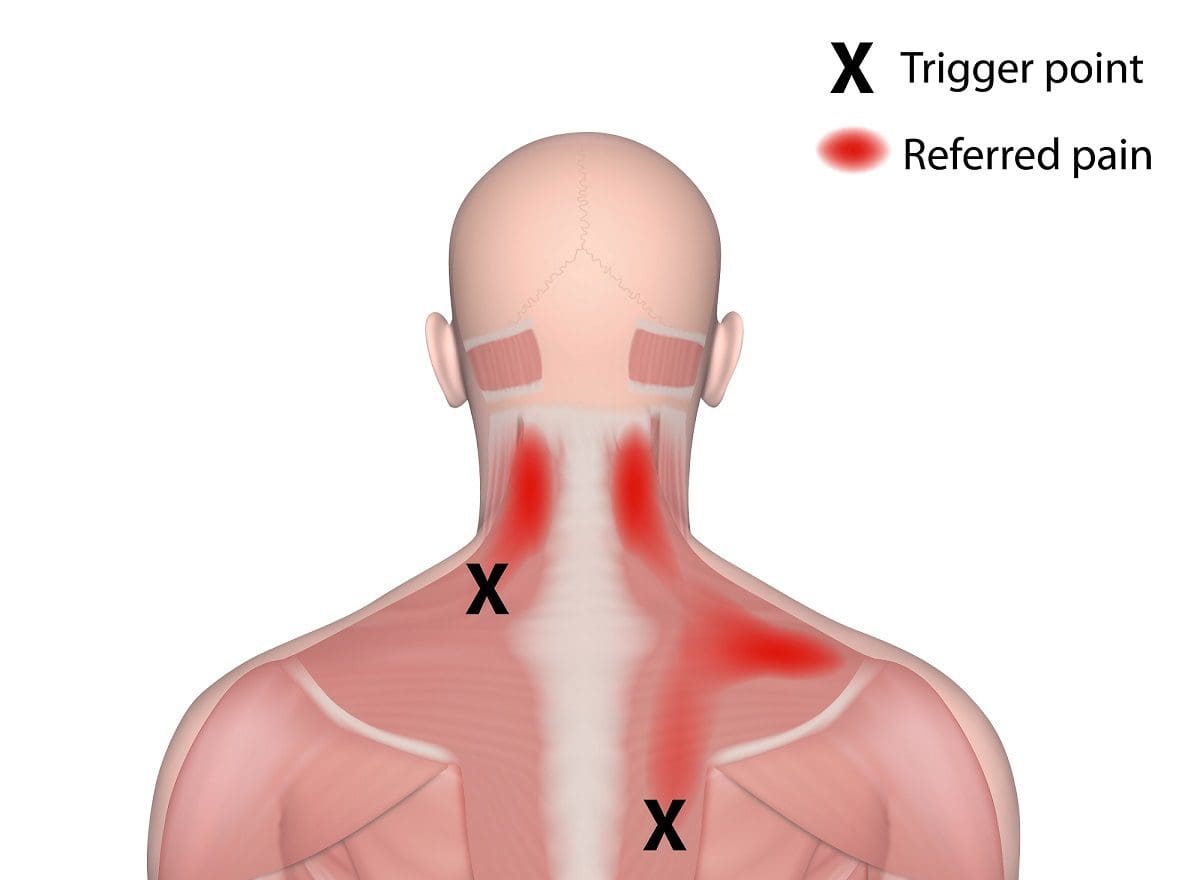
Have you been experiencing muscle tightness in different areas of your body? Have you felt your muscles tender to the touch? Or have you been having trouble sleeping? Many of these overlapping risk factors are signs that you might have myofascial pain syndrome. The term “myofascial” is split into two parts. “Myo” refers to the muscles, while “fascia” refers to the connective tissues found throughout the body. So myofascial pain syndrome is where there is muscle pain in various forms, which includes the muscle tissues, connective tissues, or both. Studies reveal that myofascial pain syndrome originates from trigger points in the skeletal muscle, causing the affected muscle to be in pain. The trigger points in the body’s skeletal muscles are the “knots” people feel when their muscles feel tight. These trigger points are challenging to identify because they occur in different areas causing referred pain (pain in one place but in another body area).
How Central Sensitization Link To Myofascial Pain Syndrome?
Studies reveal that central sensitization in the body is represented as an enhancement in neuron function and circuits in the nociceptive pathways that increases membrane excitability and synaptic efficacy. To that point, it reduces inhibition and manifests the remarkable plasticity of the somatosensory nervous system. The nociceptor inputs can trigger and manifest central sensitization as pain hypersensitivity when the body suffers from an injury. So how is central sensitization linked to myofascial pain syndrome? Let’s use fibromyalgia as an example. Many individuals dealing with myofascial pain may be potentially involved with fibromyalgia. This is due to fibromyalgia being a chronic condition that features widespread pain, and this causes the body to be more sensitive to pain. Central sensitization linked to myofascial pain syndrome can mimic fibromyalgia symptoms in the body, causing muscle pain and discomfort.
An Overview Of Myofascial Pain Syndrome-Video
Are you experiencing muscle weakness or soreness in some regions of your body? Have you dealt with chronic fatigue or poor sleep quality? Or have you been dealing with headaches constantly throughout the entire day? Many of these symptoms are signs that you might be at risk of developing myofascial pain syndrome. The video above explains myofascial pain syndrome, the symptoms, and the causes that affect the body. Studies reveal that myofascial pain has two types of trigger points:
- Active trigger points associated with muscle pain without movement
- Latent trigger points associated with muscle pain with movement
Myofascial pain syndrome can vary in acute or chronic forms and can range from mild to severe while being in different locations, making it very difficult to pinpoint where the pain is localized. Fortunately, there are ways to manage myofascial pain syndrome in the body that can help with the pain.
Ways To Manage Myofascial Pain Syndrome
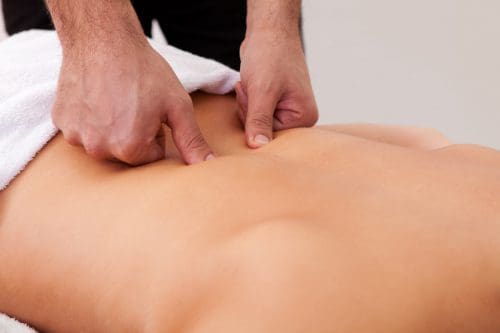
When managing myofascial pain syndrome, many individuals dealing with muscle pain will take pain medication to alleviate it; however, that only minimizes the pain for a short period. One way to manage myofascial pain syndrome is by utilizing chiropractic care as part of treatment. Chiropractic care is non-invasive and often the preferred treatment for individuals with myofascial pain syndrome due to its effectiveness and drug-free approach. Chiropractors are not only good at finding the trigger points, but they are good when it comes to treating them using various techniques. Studies reveal that chiropractors use direct pressure on the trigger points to relieve the pain with their hands or specific tools. Incorporating chiropractic care provides the body with an increase in muscle strength, flexibility, and range of motion. Since chiropractic care is a whole-body approach, it allows many people with myofascial pain syndrome to have a better quality of life and learn healthy habits, which include diet, exercise, and mental health, while living with less or no pain at all.
Conclusion
The body has muscles, tissues, and ligaments that help stabilize the joints and structure of the body, so there is functionality. These muscles help facilitate movement since the muscles are interwoven in the spine and joints. When the body suffers from a traumatic event or an injury, the muscles, tissues, and ligaments become affected. This causes muscle pain and discomfort, known as myofascial pain, where the trigger points cause pain in the body and can occur in different areas. Myofascial pain can be challenging to diagnose since it can be on one side of the body but affects a different section, known as referred pain. Fortunately, treatments like chiropractic care can help manage myofascial pain by treating the pain and using direct pressure to alleviate the pain. Incorporating chiropractic care to manage myofascial pain can help many individuals be pain-free on their health and wellness journey.
References
Bordoni, Bruno, et al. “Myofascial Pain – Statpearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 18 July 2022, https://www.ncbi.nlm.nih.gov/books/NBK535344/.
Desai, Mehul J, et al. “Myofascial Pain Syndrome: A Treatment Review.” Pain and Therapy, Springer Healthcare, June 2013, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4107879/.
Latremoliere, Alban, and Clifford J Woolf. “Central Sensitization: A Generator of Pain Hypersensitivity by Central Neural Plasticity.” The Journal of Pain, U.S. National Library of Medicine, Sept. 2009, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2750819/.
Morgan, William. “Chiropractic Treatment for Myofascial Pain Syndrome.” Spine, Spine-Health, 24 Sept. 2014, https://www.spine-health.com/treatment/chiropractic/chiropractic-treatment-myofascial-pain-syndrome.
Disclaimer
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


Comments are closed.