Table of Contents
Do you feel:
- Shaky, jittery, or have tremors?
- Stomach pain, burning, or aching 1-4 hours after eating?
- Agitated, easily upset, nervous?
- Lightheaded if meals are missed?
- Digestive problems subside with rest and relaxation?
If you are experiencing any of these situations, then you might be experiencing a histamine attack on your immune system.
During an allergic response, the body’s immune system starts to react by releasing various immune compounds to protect itself from foreign substances that identify as harmful. One of these immune compounds, known as histamine, is commonly present in a variety of foods. When histamine is elevated in the body, it is due to a high dietary intake or an inability to break it down, so individuals may experience allergic symptoms from a histamine reaction.
What is Histamine?
Histamine is a compound that is formed through the metabolism of specific amino acids in the immune system. There are a variety of levels of histamine that is found naturally in the foods that people consume. It is also produced by the body where it is in specific immune cells, including mast cells and basophils. During an allergic and other immune response, histamine is released from these cells, and consuming large quantities of histamine that is over 100 mg may result in a mild adverse reaction. Studies have shown that if histamine is consumed in a higher amount that is over 1000 mg, it can lead to histamine intoxication or histamine poisoning.
What is Histamine Intolerance?
Under normal conditions, histamine is released in the body or ingested through food, and it is broken down by two enzymes: HNMT (histamine-N-methyltransferase) and DAO (diamine oxidase). High levels of histamine can occur in individuals that have reduced activity of these enzymes. When histamine levels are increased, or the ability to break down histamine is impaired, individuals may experience histamine intolerance, which will generally present itself as an allergic reaction to the immune system.
What Causes Histamine Intolerance?
Specific individuals may have an increased sensitivity to biogenic amines like histamine. Some factors have been associated with an increased risk of histamine intolerance, including:
- Gastrointestinal conditions (Crohn’s disease, gastric and colon ulcers, gastritis, irritable bowel syndrome)
- Certain health conditions (coronary heart disease, hypertension, respiratory diseases)
- Vitamin B12 deficiency
- Certain medications that inhibit the activity of histamine-degrading enzymes (acetylcysteine, metamizole, metoclopramide, metronidazole, verapamil)
Mast cell conditions can increase the secretion of histamine. Since mast cells are found throughout the body, they are involved with the innate immune response as well as being the primary source of histamine in the intestines. Studies show that when specific immune receptors detect a foreign substance in the body, the mast cells secrete inflammatory compounds like histamine as a protective response. Mast cell activation is characterized by increasing plasma and urine histamine levels as well as an increased histamine metabolite in the urine. Several conditions are associated with mast cell activation, including:
- Allergies that are mediated by IgE (immunoglobulin-E) and other hypersensitivities
- Atopic conditions
- Mastocytosis
- Primary mast cell disorders
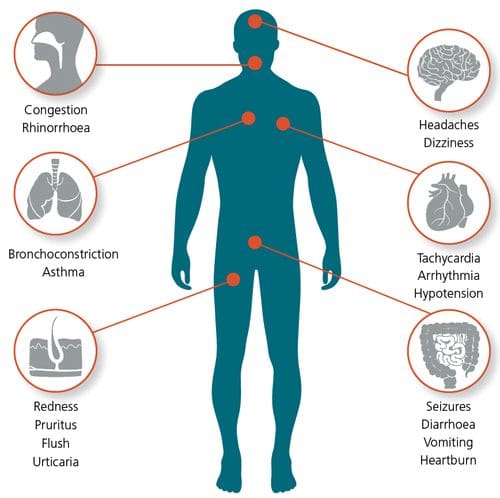
Signs and Symptoms of Histamine Intolerance
With histamine intolerance symptoms being presented as an allergic response, some of the signs and symptoms include:
- Arrhythmia
- Asthma
- Diarrhea
- Flushing
- Headaches
- Hypotension
- Symptoms of rhinoconjunctivitis (nasal congestion, post-nasal drip, sneezing)
- Pruritus (itchy skin)
- Urticaria (hives)
Histamine-free Diet
With dietary support for histamine intolerance, it may involve a histamine-free diet. Studies have been examining the effects of four-week histamine-free diet intervention on 22 individuals that have CU (chronic urticaria). Chronic urticaria is a common skin condition that is characterized by episodes of red marks and swelling that last longer than six weeks on the body.
A study found that when it is being compared to baseline, plasma histamine levels were significantly reduced when following the diet. Additionally, USS (urticaria severity score) and (UAS), both decreased following the intervention. It means that a histamine-free diet may help improve symptoms that are associated with dietary histamine intake or histamine intolerance like chronic urticaria in the body.

Research also shows that when individuals follow a histamine-reduced diet, it may increase the levels of the DAO enzyme. Research also demonstrated that when individuals followed the histamine-reduced diet for an average of 13 months, the increased levels of DAO were correlated with the degree of compliance to the diet. When high-histamine and histamine-liberated foods are eliminated, the individual’s tolerance levels can be determined by slowly reintroducing foods to test for potential reactions.
Certain foods may increase histamine levels by providing a dietary source or by liberating histamine in the body. Studies have found that it is essential to note that inconsistent levels of histamine are found in various foods and that the levels may fluctuate based on the maturity, storage, and processing of the food.
Here are the high-histamine foods to avoid on a histamine-free diet. They are:
- Aged cheese (cheddar, gouda, parmesan)
- Alcohol (beer, champagne, wine)
- Certain produce (avocado, eggplant, spinach, tomato)
- Cured meats (fermented sausage, salami)
- Fermented vegetables (sauerkraut)
- Fish products (dried anchovies, fish sauce)
Here are the histamine-liberating foods to avoid on a histamine-free diet as well. They are:
- Certain fruits (citrus, pineapple, banana, strawberries, papaya)
- Cocoa
- Egg whites
- Food additives (coloring, flavoring, preservatives, stabilizers)
- Legumes
- Licorice
Other Considerations
With methods surrounding food preparations that should be considered, researchers have suggested that people should consume food that is fresh as possible and boiled rather than frying or grilling food may help reduce the intake of biogenic amines like histamine. Studies have shown that spoiled foods have been found to have high levels of histamine, so it is essential to be mindful when consuming leftovers, especially leftover fish. There are some individuals with histamine intolerance that may benefit from taking antihistamine medication or a DAO supplement. There are also certain nutrients, including copper, vitamin B6, and vitamin C that can help support histamine degradation.
Conclusion
When the body is suffering from an allergic response, its’ immune system starts to react by sending out various immune compounds that attack harmful foreign substances. Histamine is one of the immune compounds that is produced and broken down to HNMT and DAO. Histamine can also trigger an asthma attack on individuals, while certain foods can contain high-histamine and histamine-liberating properties that can be harmful in the body. Some products use an advanced formula that helps support the immune system, targets amino acids, and supports antioxidant processes to make sure that the body is functioning correctly.
The scope of our information is limited to chiropractic, musculoskeletal, and nervous health issues or functional medicine articles, topics, and discussions. We use functional health protocols to treat injuries or disorders of the musculoskeletal system. Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. To further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900.
References:
Martin, San Mauro, et al. “Histamine Intolerance and Dietary Management: A Complete Review.” Adrianaduelo, 31 Aug. 2016, www.adrianaduelo.com/wp-content/uploads/2016/09/2016_Histamine-intolerance-and-dietary-management.pdf.
Chung, Bo Young, et al. “Effect of Different Cooking Methods on Histamine Levels in Selected Foods.” Annals of Dermatology, The Korean Dermatological Association; The Korean Society for Investigative Dermatology, Dec. 2017, www.ncbi.nlm.nih.gov/pmc/articles/PMC5705351/.
Dougherty, Joseph M. “Allergy.” StatPearls [Internet]., U.S. National Library of Medicine, 28 July 2019, www.ncbi.nlm.nih.gov/books/NBK545237/.
Fong, Michael. “Histology, Mast Cells.” StatPearls [Internet]., U.S. National Library of Medicine, 20 Sept. 2019, www.ncbi.nlm.nih.gov/books/NBK499904/.
Lackner, Sonja, et al. “Histamine-Reduced Diet and Increase of Serum Diamine Oxidase Correlating to Diet Compliance in Histamine Intolerance.” European Journal of Clinical Nutrition, U.S. National Library of Medicine, Jan. 2019, www.ncbi.nlm.nih.gov/pubmed/30022117.
Maintz, Laura, and Natalija Novak. “Histamine and Histamine Intolerance.” OUP Academic, Oxford University Press, 1 May 2007, academic.oup.com/ajcn/article/85/5/1185/4633007.
Reese, Imke, et al. “German Guideline for the Management of Adverse Reactions to Ingested Histamine: Guideline of the German Society for Allergology and Clinical Immunology (DGAKI), the German Society for Pediatric Allergology and Environmental Medicine (GPA), the German Association of Allergologists (AeDA), and the Swiss Society for Allergology and Immunology (SGAI).” Allergo Journal International, Springer Medizin, 2017, www.ncbi.nlm.nih.gov/pmc/articles/PMC5346110/.
Son, Jee Hee, et al. “A Histamine-Free Diet Is Helpful for Treatment of Adult Patients with Chronic Spontaneous Urticaria.” Annals of Dermatology, The Korean Dermatological Association; The Korean Society for Investigative Dermatology, Apr. 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC5839887/.
Sánchez-Pérez, Sònia, et al. “Biogenic Amines in Plant-Origin Foods: Are They Frequently Underestimated in Low-Histamine Diets?” Foods (Basel, Switzerland), MDPI, 14 Dec. 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC6306728/.
Unknown, Unknown. “Histamine Intolerance & Diet: What You Should Know.” Fullscript, 11 Nov. 2019, fullscript.com/blog/histamine-intolerance.
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



Comments are closed.