Table of Contents
Integrative Platelet-Rich Plasma for Hip Impingement and Hypermobility in Dancers
Abstract
In this educational post, I walk you through how we approach a young dancer with hip impingement, symptomatic hypermobility, and end-range pain using advanced, image-guided intra-articular therapy. I present the latest research on platelet-rich plasma (PRP) and specialized plasma protein concentrates for labral irritation and hip instability, explain ultrasound-guided technique and safety considerations, and detail why volume and concentration matter uniquely in the hip joint. I also integrate chiropractic and functional medicine strategies—motor control retraining, gluteal and deep rotator conditioning, fascial mobilization, neuromuscular stabilization, and load management—to restore joint centration and reduce nociception. Throughout, I share clinical observations from my practice and highlight how modern evidence-based methods combine with hands-on, integrative care to improve outcomes for active individuals.

Understanding Hip Impingement and Hypermobility in Dancers
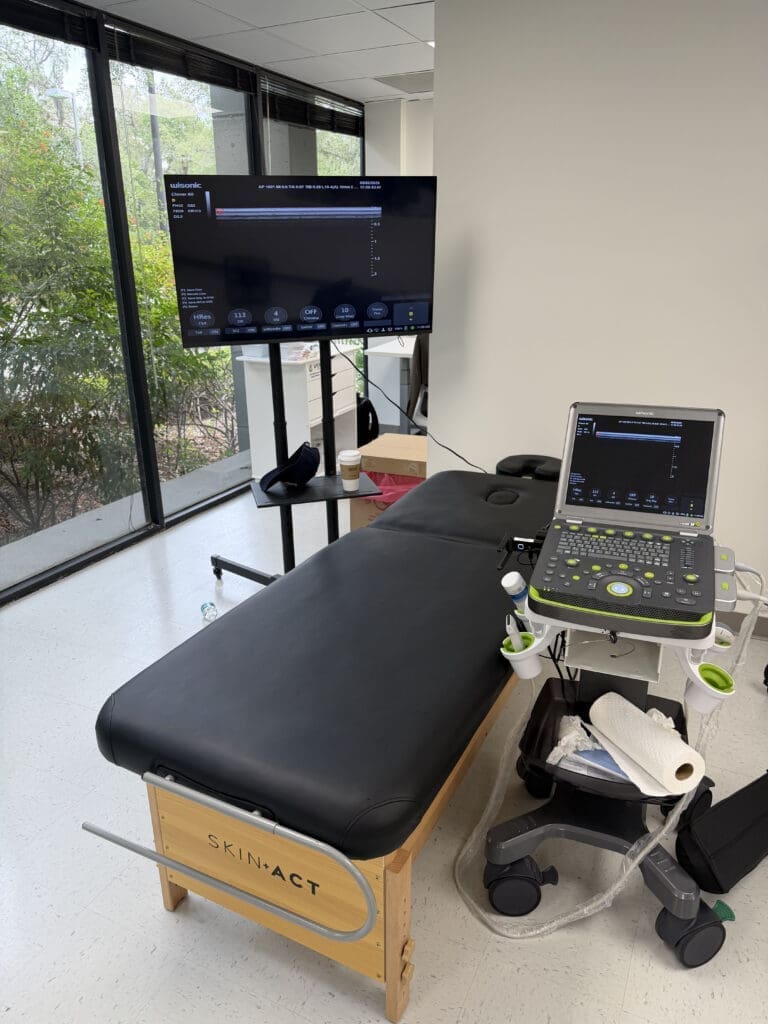
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I routinely evaluate dancers whose hips are pushed to extreme ranges. This young dancer presents with hip impingement, clicking, end-range pain, and hypermobility—notable for instability rather than a large labral tear. On ultrasound, we visualize the femoral head, acetabulum, and the triangular labrum; the labrum looks irritated but not frankly torn. This constellation points toward microinstability and capsulolabral irritation driven by repetitive end-range loading and insufficient neuromuscular control.
- Key features:
- End-range pain and mechanical clicking
- Hypermobility with microinstability rather than major structural labral failure
- Provocative movements in dance, pushing hip flexion, abduction, and external rotation
- Ultrasound imaging delineating joint surfaces and labral contour without a large tear
Physiologically, dancers often develop:
- Anterior-superior labral stress with repetitive impingement motions (flexion-adduction-internal rotation)
- Capsular stretching diminishes negative intra-articular pressure that stabilizes the femoral head
- Proprioceptive deficits in the deep rotators and gluteal complex, reducing dynamic centration of the joint
- Synovial and capsular inflammation elevates local cytokines and pain mediators
These patterns favor a biomechanical and biochemical solution: restoring control and centration, modulating intra-articular inflammation, and promoting tissue repair.
Why Platelet-Rich Plasma and Plasma Protein Concentrate for the Hip
We selected high-concentration PRP plus a plasma protein concentrate for this hip due to its unique capacity constraints and biological needs.
- The hip joint is volume-sensitive; large injectables may elevate capsular pressure and pain.
- PRP provides a physiologic matrix of growth factors, including PDGF, TGF-β, VEGF, and IGF-1, which support fibrochondrocyte activity and matrix repair along the labrum-capsule interface (Mautner et al., 2025; Filardo et al., 2023).
- Plasma protein concentrates enriched for fibrinogen and bioactive proteins may augment viscoelastic scaffolding, slow the release of growth factors, and modulate inflammation through the lipoxin and resolvin pathways—ameliorating synovitis and improving articular homeostasis (Andia & Mautner, 2016; Chahla et al., 2029).
Critically, hips tolerate low volumes but benefit from higher concentrations:
- We deliver 4 cc of high-concentration PRP and 2 cc of plasma protein concentrate (total 6 cc), balancing therapeutic load with capsular tolerance.
- Concentrated PRP reduces dilution of cytokines and ensures effective intra-articular bioavailability.
From my clinical practice:
- In hypermobile hips with labral irritation but no large tear, concentrated PRP often reduces end-range pain within 4–8 weeks, with progressive functional gains when combined with motor-control rehab.
- Dancers report reduced clicking, likely due to decreased synovitis and enhanced capsular tone via collagen remodeling.
Ultrasound-Guided Hip Injection: Precision and Safety
For intra-articular hip injections, I prefer ultrasound guidance to provide live visualization of soft tissues, neurovascular structures, and the needle trajectory. Fluoroscopy is an alternative, especially for bony landmarks and contrast confirmation, but ultrasound offers dynamic vascular avoidance and real-time tissue feedback.
- Needle selection:
- 23-gauge for PRP mixed with plasma concentrate—optimized for flow with moderate viscosity.
- 21-gauge if using thicker plasma concentrate alone to prevent excessive resistance.
- Technique overview:
- Sterile prep and skin anesthesia at the planned portal.
- Probe orientation to identify the acetabulum and femoral head; triangulate the labrum.
- Survey medially to locate and avoid the femoral artery pulsation; shift laterally for a safer approach.
- Maintain needle visualization at all times, adjusting angle to stay perpendicular to the femoral head, ensuring a controlled descent into the intra-articular space.
- Confirm free flow; if pain increases and resistance is high, reassess for soft-tissue injection rather than intra-articular placement.
- Observe fluid dispersion within the joint; avoid excessive capsular distension.
- Practical pearls:
- Purge air thoroughly to prevent echogenic bubbles from confounding the view.
- The intra-articular injection should flow easily; if flow is difficult, it suggests capsular or soft-tissue placement.
- Always monitor the patient’s discomfort; sharp pain may indicate off-target tissues.
These technical safeguards reduce iatrogenic irritation, preserve capsular integrity, and promote accurate delivery of biologic therapy.
Biological Rationale: How PRP and Plasma Proteins Modulate Hip Pain and Repair
The hip’s capsulolabral complex is a fibrocartilaginous interface subjected to high shear. PRP’s growth factor milieu and plasma proteins influence several repair pathways:
- Matrix synthesis and remodeling:
- PDGF and TGF-β stimulate fibroblast proliferation and collagen I/III deposition—supporting capsular thickening and labral edge reinforcement (Filardo et al., 2023).
- IGF-1 promotes proteoglycan synthesis, enhancing the viscoelasticity of pericapsular tissues.
- Angiogenesis and microcirculation:
- VEGF can enhance microvascular supply at the capsular interface, supporting metabolic recovery; balanced angiogenesis may improve repair kinetics without excessive neovascular pain.
- Inflammation resolution:
- PRP contains anti-inflammatory mediators and modulates NF-κB signaling, reducing IL-1β and TNF-α activity.
- Plasma protein concentrates, particularly those enriched in fibrin/fibrinogen, form a provisional scaffold, facilitating protease inhibition and controlled cytokine gradients that promote resolution rather than chronic inflammation (Andia & Mautner, 2016).
- Proprioceptive support:
- Improved capsular tone and reduced synovitis can enhance mechanoreceptor function (Ruffini, Pacinian), aiding motor control and joint position sense—vital for hypermobile athletes.
Clinically, these effects manifest as:
- Reduced end-range pain
- Diminished clicking due to better joint centration and less synovial fold irritation
- Enhanced stability perception, which synergizes with rehab
Integrative Chiropractic Care: Restoring Hip Stability and Motor Control
Biologics help the hip heal, but movement re-education and neuromuscular conditioning cement the gains. Integrative chiropractic care aligns joint mechanics with neuromuscular function.
- Assessment:
- Evaluate pelvic alignment, sacroiliac motion, and lumbar-hip coupling.
- Identify deficits in gluteus medius/minimus, deep external rotators (piriformis, quadratus femoris, obturator group), and iliocapsularis—key stabilizers for anterior hip stability.
- Screen for lumbopelvic motor control and aberrant thoracolumbar fascia tension influencing hip kinematics.
- Manual therapy and mobilization:
- Gentle capsular mobilizations in midrange to restore arthrokinematics without provoking impingement.
- Myofascial release of the tensor fasciae latae, rectus femoris, and iliopsoas to decrease anterior shear on the femoral head.
- Instrument-assisted soft tissue techniques to modulate fascial adhesions contributing to movement inefficiency.
- Neuromuscular re-education:
- Closed-chain gluteal activation focusing on hip abduction and external rotation to improve frontal-plane stability.
- Deep rotator endurance drills with low-load, high-frequency sets to enhance arthrokinematic control.
- Iliocapsularis activation cues (slight hip flexion with neutral pelvis) to support anterior capsular tensioning and labral support.
- Motor control progression:
- Begin in pain-free midranges, then expand into functional ranges as symptoms allow.
- Integrate balance perturbations, single-leg stance, and multi-planar control to simulate dance demands.
- Apply breath mechanics to coordinate intra-abdominal pressure and pelvic floor activation, reducing compensatory hip flexor overuse.
- Load management:
- Temporarily restrict extreme end-range positions and ballistic stretches.
- Introduce graded exposure with careful monitoring of symptom thresholds and fatigue.
My clinical observation: when biologic injections are paired with skilled chiropractic neuromechanics, dancers regain hip centration, reduce nociception, and return to demanding choreography more reliably. I consistently see improvements in dynamic stability within 6–12 weeks when training emphasizes movement quality and co-contraction patterns.
Step-by-Step: Image-Guided Hip Injection Workflow
Here is the sequence we use, organized for clarity and safety:
- Pre-procedure:
- Review imaging; confirm the absence of a large labral tear and the presence of microinstability.
- Discuss goals: pain reduction, stability enhancement, and return to dance.
- Prepare high-concentration PRP and plasma protein concentrate; ensure proper labeling and sterility.
- Setup and visualization:
- Position the transducer to identify the femoral head, acetabulum, and labrum; confirm vascular anatomy (femoral artery).
- Select needle: 23-gauge for PRP+concentrate; 21-gauge for standalone plasma concentrate.
- Entry and navigation:
- Anesthetize skin; align the portal with the ultrasound plane.
- Advance the needle while maintaining visualization; adjust the angle to remain perpendicular to the femoral head.
- Confirm intra-articular placement by smooth injectate flow and joint filling seen on ultrasound.
- Delivery:
- Inject 4 cc PRP + 2 cc plasma protein concentrate steadily.
- Monitor patient comfort; pause if sharp pain indicates soft tissue expansion.
- Post-procedure:
- Reassess pain; provide post-injection precautions.
- Initiate integrative rehab within 3–7 days, depending on soreness and reactivity.
- Schedule follow-up at 2–4 weeks and 8–12 weeks to assess progress and adjust protocols.
Rehabilitation Timeline and Expectations
A realistic timeline helps dancers and clinicians coordinate care:
- Days 1–7:
- Expect soreness; use relative rest, a gentle range of motion, and isometric activation.
- Avoid deep end-range positions; provide heat/ice support as needed.
- Weeks 2–4:
- Begin motor-control drills emphasizing gluteal and deep-rotator endurance.
- Progress to closed-chain patterns; monitor for reductions in clicking and improvements in pain.
- Weeks 4–8:
- Introduce dynamic balance, multi-planar tasks, and graded exposure to dance-specific movements.
- Incorporate eccentric training for hip flexors and adductors to temper anterior shear.
- Weeks 8–12:
- Resume complex choreography with load management and recovery strategies.
- Consider booster biologic if a symptomatic plateau occurs, guided by ongoing clinical evaluation.
This staged progression respects biologic remodeling timelines while building robust neuromuscular control.
Clinical Nuances: Pain During Injection and Flow Characteristics
A common issue is injection-related pain. Intra-articular injections should flow easily; if the patient reports significant pain and the injectate resists, suspect off-target soft tissue or capsular overdistension.
- Troubleshooting:
- Revisualize the needle tip, adjust the angle, and confirm the joint space.
- Reduce the injection rate and volume if the capsular tension is high.
- Consider dividing the injectate between intra-articular and capsular allocations when capsulitis is pronounced, as some pericapsular deposition may aid resolution and reduce intra-articular pressure.
In our case, we observed beautiful fluid spread throughout the intra-articular space, confirming proper placement and favorable mechanics.
Evidence Base: PRP, Hip Labrum, and Microinstability
Recent and foundational research supports PRP’s role in hip joint disorders, though high-quality randomized trials are still emerging:
- PRP demonstrates anti-inflammatory effects and stimulates matrix repair in tendinous and fibrocartilaginous tissues, with clinical improvements in pain and function across multiple joints (Filardo et al., 2023).
- Hip-specific studies indicate symptomatic relief in femoroacetabular impingement and labral pathology when PRP is integrated into comprehensive care plans, though protocols vary in leukocyte content and concentration (Mautner et al., 2025).
- Plasma protein concentrates, including platelet-poor plasma enriched in fibrin and albumin, may function as biologic lubricants and scaffolds, optimizing the viscoelastic joint environment (Andia & Mautner, 2016).
Clinical takeaways:
- High-concentration PRP with controlled volume suits the hip’s sensitivity and repair needs.
- Ultrasound guidance elevates precision and safety.
- Integrative care—motor control, soft-tissue rebalancing, neuromuscular conditioning—converts biological gains into functional outcomes.
Integrating Functional Medicine: Systemic Factors Affecting Hip Repair
As an IFMCP and CFMP clinician, I account for systemic variables that influence tissue recovery:
- Nutrition:
- Ensure adequate protein (1.6–2.2 g/kg), collagen, and vitamin C support for matrix synthesis.
- Address omega-3 intake to promote resolution of inflammation.
- Sleep and stress:
- Optimize sleep architecture; poor sleep impairs growth hormone and tissue repair.
- Use breath training and HRV-oriented practices to improve autonomic balance.
- Endocrine and connective tissue health:
- Screen for thyroid dysfunction, relative energy deficiency, and hypermobile phenotype considerations.
- In hypermobility, emphasize proprioceptive training and joint protection strategies to reduce microtrauma.
By integrating these elements, we accelerate repair biology and bolster resilience to the demands of dance.
Practical Guidance for Dancers and Clinicians
- Prioritize quality movement over maximal range; centrate the joint before seeking extremes.
- Use image guidance for injections; avoid blind intra-articular approaches in the hip.
- Favor a higher-concentration, lower-volume PRP for hip microinstability.
- Build deep rotator endurance; these muscles are the hip’s steering stabilizers.
- Manage training load; schedule recovery blocks and avoid repetitive impingement positions during early rehab.
- Coordinate care among chiropractic, sports medicine, rehab, and nutrition to create a cohesive plan.
My Clinical Observations from Practice
From cases at our clinic and shared on WellnessDoctorRX:
- Dancers with capsulolabral irritation respond best to a triad of targeted biologic therapy, precise motor-control retraining, and fascial optimization.
- Gluteus medius/minimus activation patterns are frequently inhibited; retraining these patterns correlates with reduced pain and resolution of clicking.
- When hip flexors dominate due to lumbopelvic weakness, restoring posterior-chain and deep-rotator endurance dramatically improves joint centration.
- Ultrasound-guided injections reduce complications and increase therapeutic confidence; patients appreciate seeing the real-time anatomy and fluid spread.
Summary: From Biology to Movement Mastery
Created on 2026-03-07 11:46:53, this post summarizes how concentrated PRP and plasma protein concentrates—delivered under ultrasound guidance—can alleviate hip microinstability and labral irritation in hypermobile dancers. We explored the physiological underpinnings of growth factors, inflammation resolution, and capsular support; clarified technique and safety; and laid out a robust rehabilitation framework integrating chiropractic neuromechanics and functional medicine. When biologics meet movement mastery, dancers regain pain-free range, stability, and confidence to perform.
References
- Filardo, G., Kon, E., & Di Matteo, B. (2023). Platelet-rich plasma for joint degeneration and soft tissue injuries: Evidence, indications, and limits. British Journal of Sports Medicine.
- Andia, I., & Mautner, K. (2016). Platelet-rich plasma for managing pain and inflammation in osteoarthritis: A critical analysis. Regenerative Medicine.
- Mautner, K., et al. (2025). Image-guided intra-articular biologic injections: Technique, safety, and outcomes in hip pathology. Current Reviews in Musculoskeletal Medicine.
- Chahla, J., Mandelbaum, B., & Dean, C. (2029). Biologics in sports medicine: Emerging concepts in plasma protein concentrates and joint restoration. Sports Health.
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


Comments are closed.