Managing Gluteus Maximus Pain and Inflammation
Individuals dealing with pain in the buttocks can make life difficult to sit, walk, or perform simple, everyday tasks. Can understanding the anatomy, location, and function of the gluteus maximus muscle help in muscle rehabilitation and avoid potential injuries?
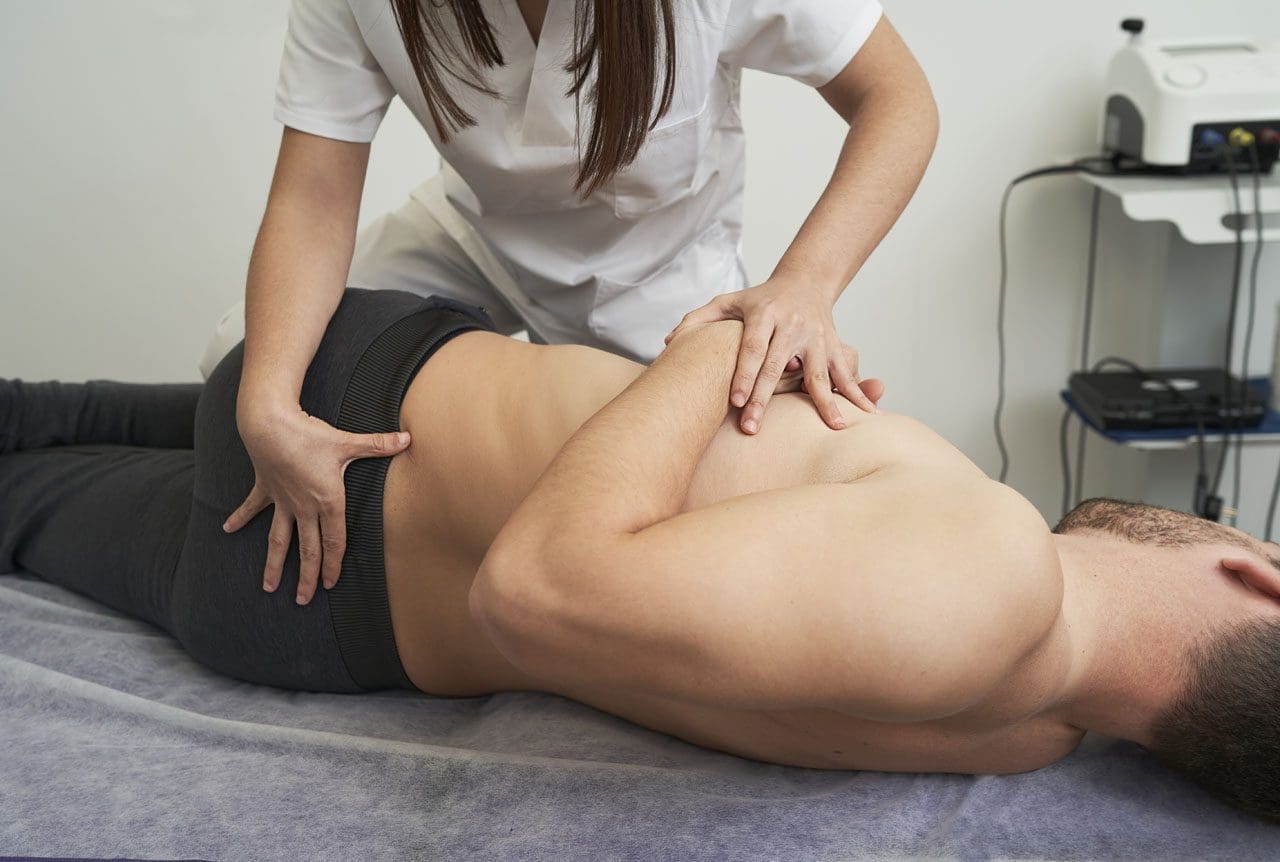
Table of Contents
Gluteus Maximus
The gluteus maximus is the largest human body muscle responsible for hip extension, external rotation, adduction, and abduction, as well as the ability to stand upright. The primary muscle extends laterally and keeps the body upright by supporting the bony pelvis and trunk. (Neto W. K. et al., 2020) When the gluteus maximus is strained, injured, or weak, it can lead to pain and inflammation.
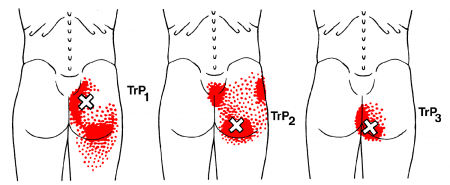
Common symptoms can include:
- Stiffness in the buttock
- Discomfort while sitting
- Difficulty standing up from sitting
- Difficulty bending over
- Pain when walking, especially upstairs or on a hill
- Pain in the lower back and/or tailbone
Anatomy and Structure
The muscles that comprise the glutes are the gluteus maximus, gluteus medius, and gluteus minimus. The gluteus medius runs underneath the gluteus maximus, and the gluteus minimus is underneath the gluteus medius.
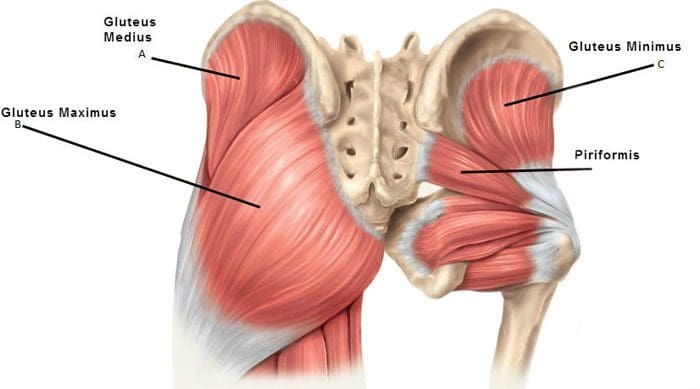
The gluteus maximus is one of the strongest muscles. Fibers from the muscle connect to different body parts, including the femur/thighbone and the iliotibial band, which comprises connective tissue that runs up the thigh. The superior gluteal artery transports blood from the heart to the glutes.
Nerve Supply
The inferior gluteal nerve, part of the sacral plexus branch, innervates the maximus muscle. The sacral plexus nerves support motor and sensory function in the thighs, lower legs, feet, and pelvis. The sciatic nerve runs under the gluteus maximus, from the lower back down to the leg, and is often the cause of nerve pain in and around the area. (Carro L. P. et al., 2016) The main nerve of the perineum is the pudendal nerve, which runs under the gluteus maximus muscle.
Location
The gluteus maximus muscle defines the buttocks. It can be called a superficial muscle, sometimes referred to muscles that help provide shape. The origin of the gluteus maximus connects to the sacrum, the ilium, or the large upper part of the hip bone, the thoracolumbar fascia tissue, and the sacrotuberous ligaments attached to the posterior superior iliac spine. The gluteus maximus has a 45-degree angle from the pelvis to the buttocks and then inserts at the gluteal tuberosity of the femur and the iliotibial tract.
Variations
Sometimes, a duplicate muscle may originate from the gluteus maximus muscle in rare cases. However, it is more common that the gluteus maximus muscle fibers may be inserted into different body parts than where they are typically inserted. (Taylor, V. G., Geoffrey & Reeves, Rustin. 2015) This can cause a condition called greater trochanteric pain syndrome or GTPS. Inflammation of the gluteus medius, minimum tendons, and bursa inflammation can also cause GTPS. Individuals with GTPS will have tenderness or a pulsing feeling on the outer side of the hip and thigh when lying on the side, along with other symptoms.
Function
The gluteus maximus extends and externally rotates the hip joint, stabilizing the body. It is highly engaged during running and hiking activities. Regular walking does not typically target gluteus maximus strength training. However, the gluteus maximus promotes balance when walking and other activities by helping keep the pelvis and posture upright.
Conditions
The most common condition associated with the gluteus maximus is muscle strain, and deep gluteus maximus syndrome is another condition that can cause pain and involves the muscles.
Muscle Strain
A muscle strain can result from stretching and working the muscle too much that it becomes overstretched or tears. (Falótico G. G. et al., 2015) This can happen from not warming up or cooling down properly, repetitive use injury, and over-exercising. Alternatively, not exercising and not utilizing your gluteus maximus can weaken it, leading to lower back pain, hip pain, and stability and posture issues. (Jeong U. C. et al., 2015)
Deep Gluteus Maximus Syndrome
This syndrome causes pain in the buttocks when the sciatic nerve becomes entrapped. (Martin, H. D. et al., 2015) The location of the pain can help healthcare providers determine where the nerve is trapped. Those with deep gluteus maximus syndrome may experience various types of discomfort, including (Martin, H. D. et al., 2015)
- Numbness and tingling in the leg
- Pain when sitting
- Pain when walking
- Pain that radiates down the back and hips and into the thigh
To diagnose the condition, a healthcare provider may perform a physical examination and various tests to rule out other conditions that can cause similar symptoms.
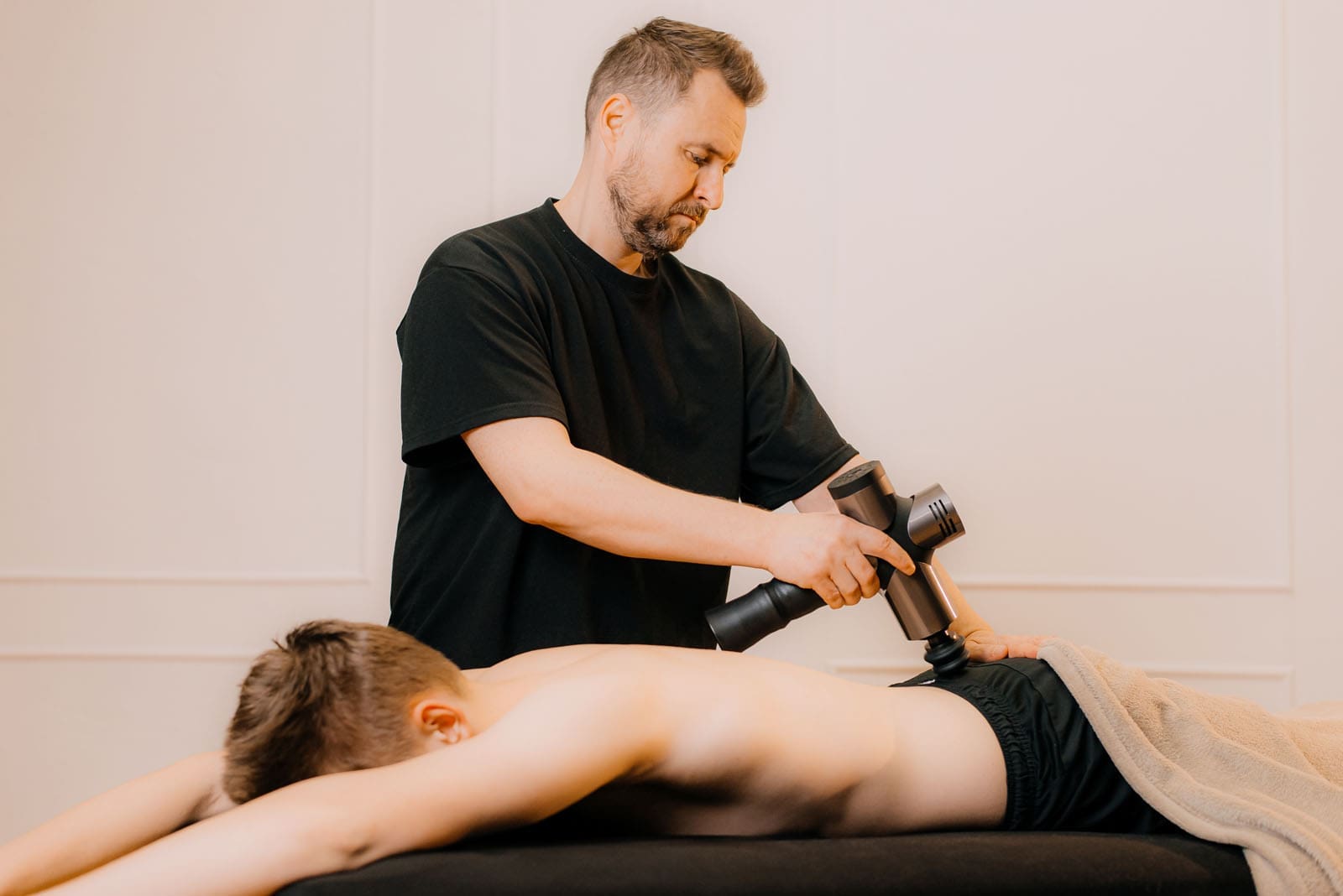
Treatment and Rehabilitation
If there is pain in the buttocks and/or lower extremities, it’s important to consult a primary doctor, chiropractor, or physical therapist. They will evaluate the strength of the gluteus muscles to diagnose any strain or weakness. From there, they will develop a personalized treatment plan to help heal the injury, strengthen the muscles, and restore function. Treatment will include stretches once the strain is rested and improves.
- Recommendations can include taking a few days off to rest the muscle or, at the very least, stop performing the work or activity that caused the strain.
- Ice and over-the-counter medication like ibuprofen can help reduce inflammation.
- For weak gluteus maximus, a physical therapist will strengthen and retrain the muscle with a tailored program of exercises. (Jeong U. C. et al., 2015)
- Treatment for deep gluteus maximus syndrome may include conservative treatment, such as chiropractic decompression and realignment, physical therapy, medications for pain and inflammation, and injections.
- If conservative treatments do not relieve the pain, a primary healthcare provider may recommend surgery. (Martin, H. D. et al., 2015)
Working with a chiropractic physical therapy team can help individuals return to normal function and expedite healing. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop a customized treatment program through an integrated approach to treating injuries and chronic pain syndromes, improving flexibility, mobility, and agility to relieve pain and help individuals return to normal activities. If other treatments are needed, Dr. Jimenez has teamed up with top surgeons, clinical specialists, medical researchers, and rehabilitation providers to provide the most effective treatments.
The Science of Motion and Chiropractic Care
References
Neto, W. K., Soares, E. G., Vieira, T. L., Aguiar, R., Chola, T. A., Sampaio, V. L., & Gama, E. F. (2020). Gluteus Maximus Activation during Common Strength and Hypertrophy Exercises: A Systematic Review. Journal of sports science & medicine, 19(1), 195–203.
Carro, L. P., Hernando, M. F., Cerezal, L., Navarro, I. S., Fernandez, A. A., & Castillo, A. O. (2016). Deep gluteal space problems: piriformis syndrome, ischiofemoral impingement and sciatic nerve release. Muscles, ligaments and tendons journal, 6(3), 384–396. https://doi.org/10.11138/mltj/2016.6.3.384
Taylor, Victor & Guttmann, Geoffrey & Reeves, Rustin. (2015). A variant accessory muscle of the gluteus maximus. International Journal of Anatomical Variations. 8. 10-11.
Falótico, G. G., Torquato, D. F., Roim, T. C., Takata, E. T., de Castro Pochini, A., & Ejnisman, B. (2015). Gluteal pain in athletes: how should it be investigated and treated?. Revista brasileira de ortopedia, 50(4), 462–468. https://doi.org/10.1016/j.rboe.2015.07.002
Jeong, U. C., Sim, J. H., Kim, C. Y., Hwang-Bo, G., & Nam, C. W. (2015). The effects of gluteus muscle strengthening exercise and lumbar stabilization exercise on lumbar muscle strength and balance in chronic low back pain patients. Journal of physical therapy science, 27(12), 3813–3816. https://doi.org/10.1589/jpts.27.3813
Martin, H. D., Reddy, M., & Gómez-Hoyos, J. (2015). Deep gluteal syndrome. Journal of hip preservation surgery, 2(2), 99–107. https://doi.org/10.1093/jhps/hnv029
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


Comments are closed.