Approximately 50 percent of the overall population will experience neck pain at some point in their lifetimes, with sports-related injuries accounting for about 10% of all neck injuries and symptoms. The cervical spine is a region which requires more concentrated attention than it usually receives. – Dr. Alex Jimenez, Chiropractor El Paso
The predominance of neck injuries in sports is believed to be rising, mostly due to the increased improvements in injury recording and observation. However, the growth of physical, extreme sports has led to higher risks of injury among unprepared athletes.
For instance, athletes who participate in sports such as skeleton, where individuals sprint on ice and hurtle head first down an icy, often bumpy track at elevated speeds, must learn to understand the importance of properly training their neck to avoid complications to its surrounding structures. Neck injuries are common in skeleton but these can be prevented. Neck training doesn’t simply involve avoiding the risk of suffering a neck complication, in competitive sports, such as skeleton, strengthening the neck can ultimately improve an athlete’s overall physical performance, helping them achieve their goals of triumph.
In order to decrease the chance of injury, the neck needs to be strategically and individually prepared to ensure it has a greater tolerance to the increased loads it’s exposed to. But, before an athlete begins implementing this program, it’s essential for them to receive an accurate evaluation of their cervical spine in a comprehensive assessment and screening process.
Table of Contents
How Neck Injuries Occur
Neck injuries occur most frequently in motorsports and high impact, collision sports like rugby. It’s been previously described that acute force exposure through compression and distraction, axial loading and/or direct blows along with sudden acceleration and deceleration of the structures of the body, are the most common reasons for injury in these types of sports.
Compression, or axial loading, is the primary means of neck injuries in sports and often results when load is applied and the neck’s natural lordosis, or curvature, is lost, generally due to an excess flexion which leads to an improper distribution of the energy placed against the body.
With acute exposure, the increased pressure can cause severe damage or injury to the cervical spine while chronic exposure can create an accumulative effect. Collapsed scrums in rugby, falls from heights and unexpectedly, timed maneuvers in combat sports can create situations where neck injuries may occur. Another type of neck injury which can develop from axial forces include brachial plexopathy irritation or injury. These can be either compressive or distractive in nature, most frequently reported among athletes who participate in tackling sports or as a result of a fall from a height where the neck is laterally flexed and the shoulder girdle is decompressed.
Brachial plexopathy injuries occur when a downward traction pressure is applied on the shoulder girdle as the neck is contra-laterally flexed or may occur due to compressive forces being placed against the vertebra of the spine. Symptoms can include temporary, altered sensations and weakness as a result of irritation to the nerve roots found along the cervical region of the spine. Following any compression or distraction injuries, healthcare professionals, including a chiropractor, should suspect the presence of spinal cord injury. This severe complication may need to be cleared by a healthcare professional following a thorough on-field assessment before the athlete is moved.
Whiplash Associated Disorders
Whiplash is a commonly diagnosed type of neck injury, most frequently caused by the sheer force of an automobile accident against the complex structures of the cervical spine, however, it can also commonly occur in sports which also involve sudden acceleration and deceleration of the body or after an athlete has suffered a direct flow to the trunk or head. A combination of neck pain, headaches, temporal mandibular dysfunction and referred pain as well as neurological symptoms may result when applied pressure is transferred to the neck, causing sudden, uncontrolled movements which may lead to damage or injury to the anterior and posterior structure of the cervical spine.
The cervical spine, or neck, isn’t only at risk of experiencing acute injuries, chronic exposure to pressure from external and internal forces from maintained static positions, such as in sports like archery, or constant exposure to gravitational or vibration forces can frequently develop neck injuries and symptoms due to overuse. The symptoms of chronic G-force exposure include neck pain as well as dizziness, disorientation, altered vision, reduced co-ordination. These symptoms can ultimately reduce an athlete’s performance, impairing their ability to properly participate in their specific sport and may place both athletes and opponents at risk of serious complications, especially when travelling at increased speeds. These symptoms are believed to appear due to a combination of reduced blood flow to the head, visual disturbances and high amounts of load being placed on the musculature of the neck.
G force should be immensely considered in contact sports where collisions between players can expose athletes to forces equivalent to those experienced during a car crash. Long term exposure to G-forces has been determined to leave athletes with an increased risk of developing vertebral disc degeneration complications. Furthermore, exposure should be observed closely.
Evaluating Neck Injuries
Before participating in any type of sport, the basic range of mobility and strength of the neck should be properly evaluated to provide baselines to a healthcare provider in order to help them determine the most appropriate sport planning treatments, similar to any other peripheral joint injury. Chiropractors specialize in musculoskeletal injuries and conditions, focusing on restoring the natural alignment of the spine and improving its strength, flexibility and mobility. A chiropractor, along with other healthcare professionals, can perform a variety of evaluations and assessments to properly diagnose the presence of a sports injury, most commonly, neck injuries.
The structure and function of the cervical spine is complex, where the vertebra primarily contribute to the varying degrees of overall neck motion. The change of orientation of every cervical vertebra, from the mid to lower cervical spine, allows for rotation, flexion and extension of the neck, however, this also isolates lateral flexion to the upper portion of the cervical spine. When a healthcare professional determines the baseline range of movement of the neck, it is also essential to understand that this can commonly decrease with age, therefore, a normal range can vary between athletes and is likely to change over an athlete’s career.
Neck Range of Motion Stretches
The most reliable standard for measuring the range of movement of the cervical spine is radiological examination but due to expense, this technique is not considered convenient among sporting environments. Many healthcare professionals can easily determine if there’s an issue with the individual’s neck range of motion and there are several reliable and inexpensive tools which can be effectively used. These include the full-circle goniometer, or simply a tape measure to record the distance between anchor points, which can be easily replicated.
The primary stabilizers of the neck are collectively known as the deep neck flexors, consisting of the longus capitus, the longus colli, the rectus capitis anterior and the rectus capitis lateralis. Without using EMG resources, these can be difficult to isolate but are most active through the commonly prescribed craniocervical flexions, or chin tuck. The most common evaluation utilized to measure the activation and endurance of the deep neck flexors is the craniocervical flexion test and are assessed using a biofeedback device. This assessment serves as a useful baseline test and can be used to acknowledge weakness and movement control dysfunctions. To perform a craniocervical flexion test, the patient lays supine while maintaining the neck in a neutral position. Then, an uninflated pressure sensor is placed behind the neck so that it borders the occiput. The cuff is inflated to 20mm Hg. The movement is described as a slow, head nodding action. The patient must attempt to sequentially target five 2mm Hg progressive pressure increases with 10 second holds.
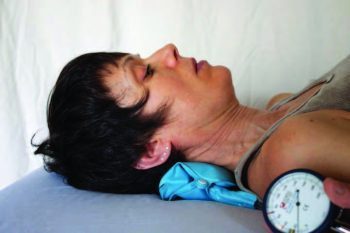
Previous studies have concluded that the activity of the stabilizers is considerably decreased and delayed in anyone with neck pain and it can be considered a great starting point for all neck rehabilitation treatments to regain stability in the structures of the cervical spine. Postural evaluations are also a key component of neck assessments. The main function of the neck is to optimize head position. Equal displacement of the weight of the head is essential when it comes to minimizing overload to the stabilizing muscles of the neck. Several tests have been developed to aid the assessment of cervical movement control dysfunctions including neck function in four-point kneeling and with upper extremity movement.
Prime Movers
Cervical prime mover strength can be evaluated in several ways including the utilization of isokinetic and isometric dynamometers which can be linked with muscle activity measurements using EMG studies. Generally, cervical extensions are stronger than flexions among popular research while lateral side flexions are commonly grouped with extensions involving a bias towards the individual’s dominant angle. Among athletes who depend on a dominant side bias, such as racquet and other throwing sport athletes, for performance advantage, this asymmetry should be understood but not necessarily be seen as detrimental.
In the case an athlete doesn’t have access to isokinetic and EMG equipment, baseline strength can be determined using a handheld dynamometer. A healthcare professional should decide on which ranges should be tested to remain consistent while accommodating any sport specific positions if necessary. To ensure all information is regulated, a healthcare professional should make sure the individual’s torso is stabilized while minimizing lower limb involvement, such as having the athlete’s feet on a wobble cushion, and appropriate ranges should be set to measure the individual’s strength through standardized warm-up and testing protocols.
The neck doesn’t function in isolation. A relationship between neck pain and shoulder dysfunction has been previously recorded through research, therefore, the entire kinetic chain should be considered when evaluating the function of the neck. Particularly among swimmers, shoulder dysfunctions can frequently lead to hypertonicity of the muscles surrounding the neck which can cause muscle imbalances, dysfunction and pain, all which could eventually lead to further neck injury in the athlete if left without a proper assessment.
Neck Injuries and Concussions
When treating acute neck injuries, healthcare professionals, or chiropractors, among others, should suspect the presence of concussions in athletes due to the increased forces that are transferred between the regions of the cervical spine. After providing the above neck evaluations, a proper assessment on athletes should be carried out to determine if there was any head trauma, or concussion, following a neck injury. Research has concluded that concussions may be associated with the strength of the neck. In fact, studies showed that neck strength is a significant predictor of concussion amongst a large percentage of high school athletes and, although further research is needed, these showed positive outcomes in reducing the risk of concussion when individuals adopt these neck strengthening programs.
In conclusion, cervical injuries can occur in a variety of sporting environments from the result of acute trauma through axial loading, prolonged position exposure, whiplash and external forces, such as vibrations and G forces. All cervical evaluations for neck injuries should rule out severe spinal injury and concussion as well as include range of movement measurements and prime mover strength assessments. 
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .
Sourced through Scoop.it from: www.elpasochiropractorblog.com
By Dr. Alex Jimenez, Chiropractor El Paso
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



Comments are closed.