PRP Therapy for Sciatica: A Regenerative Approach
Table of Contents
PRP Therapy for Sciatica: How Regenerative Treatment and Integrative Chiropractic Care May Help
Sciatica is not a diagnosis by itself. It is a pain pattern that usually happens when a lumbar disc problem irritates or compresses a nerve root in the lower back. That nerve irritation can send pain from the back into the buttock, thigh, calf, or foot. Many people also feel burning, tingling, numbness, or weakness. Because disc herniation can cause both mechanical pressure and inflammation around the nerve root, treatment often works best when it addresses both issues rather than merely blocking pain for a short time (Zhang et al., 2024; Machado et al., 2023).
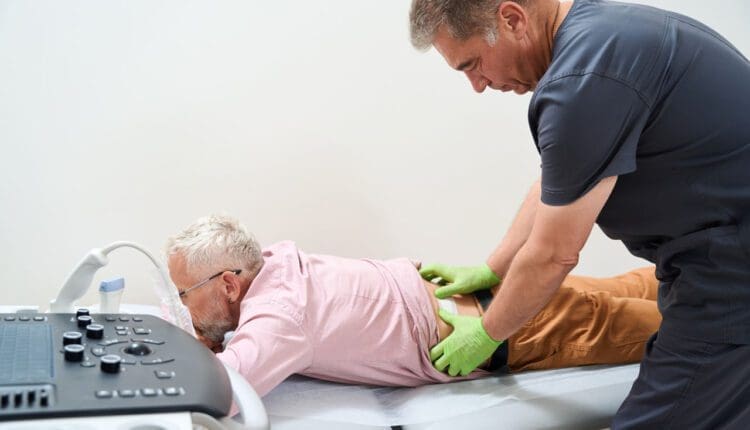
What is PRP therapy for sciatica?
Platelet-Rich Plasma, or PRP, is made from a sample of the patient’s own blood. That blood is processed so the platelet portion becomes more concentrated. When platelets are activated, they release growth factors that help regulate inflammation and support tissue repair. Reviews of lumbar spine PRP and nerve repair research describe these growth factors as part of the reason PRP has become an important regenerative medicine option in musculoskeletal care (Machado et al., 2023; Wang et al., 2024; Shang & Liu, 2025).
In simple terms, steroid injections are mainly used to calm inflammation, while PRP is designed to create a better healing environment. That does not mean PRP is a miracle fix or that every patient will regenerate a damaged disc or nerve. It means PRP is being studied as a treatment that may do more than temporarily numb the problem. Current evidence is promising but still evolving, and treatment protocols are not yet fully standardized across clinics and studies (Machado et al., 2023; Shang & Liu, 2025).
How PRP may help relieve sciatic nerve pain
Sciatica from a disc herniation often involves two overlapping problems: direct nerve root compression and a local inflammatory reaction. A major review of lumbar PRP explained that disc herniation can trigger radiculopathy through both the physical pressure of disc material and inflammatory cytokines such as TNF-alpha and IL-6. PRP is being studied because it may help calm that inflammatory environment while also supporting tissue repair in the disc and nearby nerve structures (Machado et al., 2023).
Possible ways PRP may help include:
- lowering harmful inflammation around the nerve root and disc
- delivering growth factors linked to tissue repair
- supporting disc cell activity and matrix repair
- helping create a better environment for nerve healing
- improving pain and function over time in selected patients
These effects are supported by lumbar spine reviews and nerve-repair reviews, but it is important to be honest: much of the strongest “nerve regeneration” evidence still comes from preclinical and early clinical literature, not from large standardized human trials focused only on lumbar sciatica (Machado et al., 2023; Wang et al., 2024; Shang & Liu, 2025).
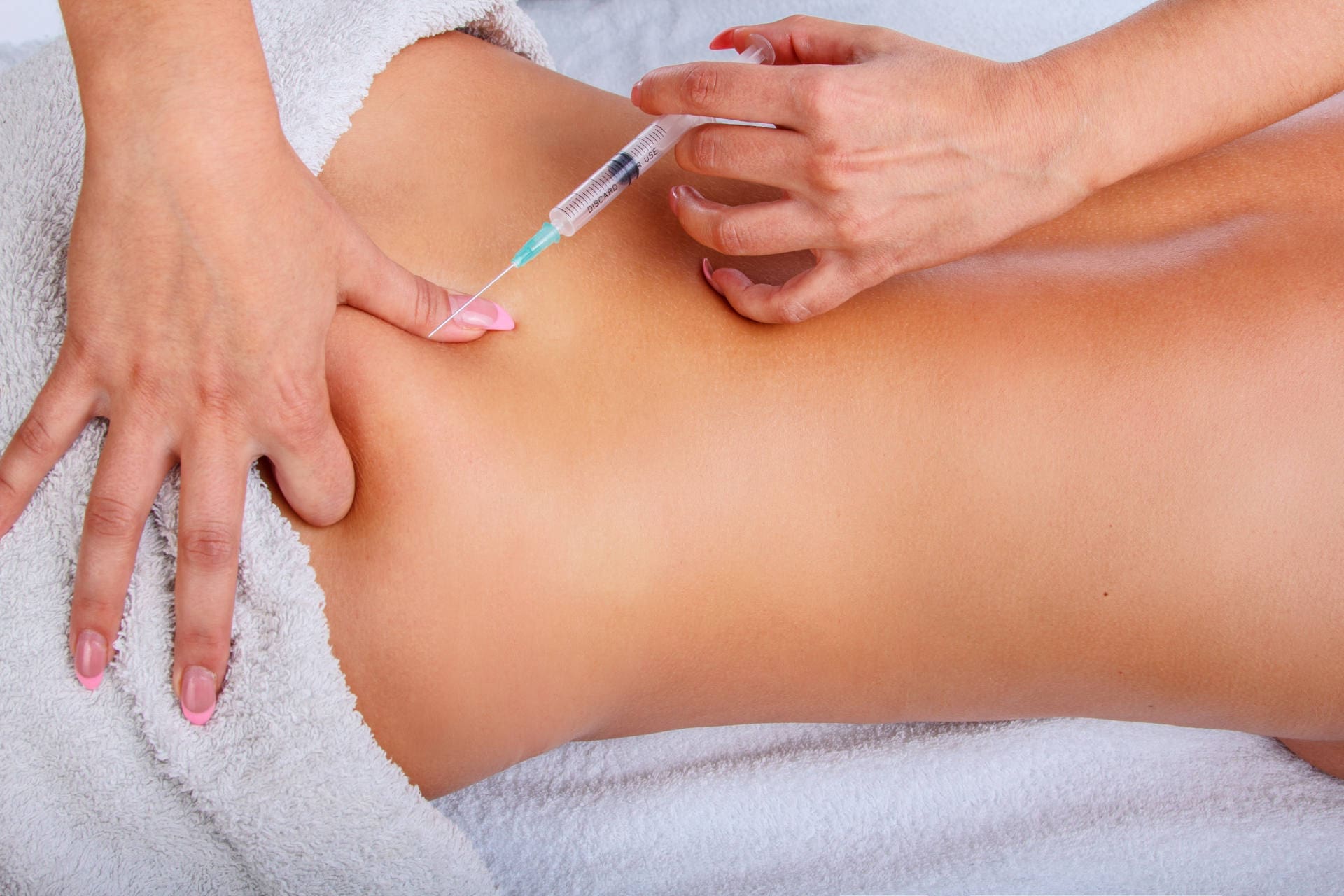
Where is PRP injected for sciatica?
The route depends on the source of pain. In lumbar radiculopathy or sciatica, a common approach is an epidural or transforaminal injection, in which PRP is placed into the epidural space near the irritated nerve root. Another method is intradiscal injection, where PRP is placed directly into a damaged disc in carefully selected cases. A broad-spectrum PRP review found evidence for both epidural and intradiscal approaches, with different studies targeting discs, the epidural space, facets, or combined pain generators (Machado et al., 2023).
That point matters because not all sciatica comes from the same structure. Some patients primarily have nerve root irritation due to a disc herniation. Others have mixed pain from disc degeneration, facet overload, inflammation, poor movement mechanics, or repeated physical strain. A reputable clinic should identify the primary pain generator before recommending PRP, rather than assuming every patient needs the same injection (Zhang et al., 2024; Machado et al., 2023).
PRP vs. steroid injections for sciatica
Epidural steroid injections are widely used and do help many patients, especially in the short term. A 2024 systematic review and meta-analysis found that epidural steroid injection improved sciatica pain in the short term (within 3 months) and the medium term (within 6 months), but long-term pain relief was limited. That same review also found no significant improvement in sciatic nerve function and noted low overall complication rates (Zhang et al., 2024).
PRP may compare favorably with longer follow-up in some smaller trials. In a 2023 randomized controlled trial, patients receiving transforaminal epidural PRP showed statistically and clinically significant improvements in leg pain at 6, 12, and 24 weeks, with no adverse events reported. In another 2023 prospective, double-blind study, both PRP and steroids provided short-term benefits, but clinically meaningful improvement lasting 6 months was observed only in the PRP group. A 2024 randomized pilot study also found that steroids were more effective at 1 week, whereas PRP showed better outcomes at later follow-up points, such as 6 weeks and 6 months (Wongjarupong et al., 2023; Saraf et al., 2023; Gupta et al., 2024).
What this means in plain language is simple:
- Steroid injections may calm pain faster
- PRP may offer slower but more durable improvement in some patients
- Both options still need careful patient selection
- PRP evidence is encouraging, but it is not yet final or uniform
That balanced reading aligns with the 2023 systematic review, which rated the overall lumbar PRP evidence as moderate, reported low adverse-event rates, and warned that study differences make direct comparison difficult (Machado et al., 2023).
Why an integrative chiropractic clinic with APRN support may matter
PRP works best when it is part of a larger plan, not a stand-alone shortcut. On his website and professional profile, Dr. Alexander Jimenez describes a multidisciplinary model built around dual licensure as a chiropractor and a family nurse practitioner, along with training in functional and integrative medicine. His published clinic materials emphasize root-cause assessment, detailed health history, rehabilitation, chiropractic care, and personalized plans rather than symptom-only treatment (Jimenez, n.d.; Jimenez, n.d./LinkedIn).
In that kind of model, a sciatica recovery plan may include the following:
- imaging and clinical testing to identify the true pain source
- chiropractic care to improve spinal motion and reduce abnormal loading
- guided exercise and rehabilitation to improve stability and movement
- PRP when a regenerative injection is a reasonable fit
- APRN or functional medicine review of inflammation, sleep, nutrition, stress, and metabolic health
- ongoing follow-up to monitor weakness, function, and recovery progress
This whole-person approach aligns with Dr. Jimenez’s published description of integrating chiropractic adjustments, functional medicine, rehabilitation, and personalized care planning for complex pain and sciatica cases (Jimenez, n.d.; Jimenez, n.d./LinkedIn).
Who may be a suitable candidate for PRP for sciatica?
A patient may be considered for PRP when symptoms fit lumbar radiculopathy, imaging and exam point to a disc-related pain source, and conservative care has not provided enough relief. In the PRP trials, patients were generally selected after failed nonoperative treatment and after matching symptoms to imaging findings. That matters because PRP is not meant to replace careful diagnosis (Wongjarupong et al., 2023; Gupta et al., 2024).
But there is another side to this discussion. Typical sciatica may cause shooting pain, tingling, numbness, and weakness. Severe or worsening weakness in both legs, numbness around the genitals or anus, or new trouble controlling urine or stool are emergency warning signs, not routine office-injection symptoms. Those signs can indicate a serious back problem, such as cauda equina syndrome, and require urgent hospital evaluation (NHS, n.d.; Cleveland Clinic, 2024).
Risks, limits, and honest expectations
PRP is usually described as low risk because it uses the patient’s own blood, and lumbar spine reviews report a low incidence of adverse events compared with similar spinal injection techniques. Still, “low risk” does not mean “no risk.” Any spinal procedure requires sterile technique, skilled imaging guidance, proper diagnosis, and realistic expectations. The research also has limitations, including small sample sizes, mixed PRP preparation methods, varied injection routes, and uneven follow-up periods (Machado et al., 2023; Shang & Liu, 2025).
A smart message for patients is this: PRP for sciatica is more than a pain shot, but it does not guarantee disc or nerve regeneration. It is best viewed as an emerging regenerative option that may help the right patient when combined with excellent biomechanics, rehabilitation, and whole-body health support. That is where an integrative clinic can add real value (Machado et al., 2023; Jimenez, n.d.).
Final thoughts
PRP therapy for sciatica is gaining attention because it may reduce inflammation, support disc and nerve healing, and provide longer-lasting relief than steroid injections for some people. The best current evidence suggests that PRP can be a meaningful option for selected patients with lumbar radiculopathy, especially when care is guided by an accurate diagnosis and combined with rehabilitation and integrative support. At the same time, the evidence is still developing, so careful patient selection and honest expectations remain essential (Zhang et al., 2024; Wongjarupong et al., 2023; Saraf et al., 2023; Machado et al., 2023).
References
Zhang, J., Zhang, R., Wang, Y., & Dang, X. (2024). Efficacy of epidural steroid injection in the treatment of sciatica secondary to lumbar disc herniation: A systematic review and meta-analysis. Frontiers in Neurology, 15, 1406504.
Machado, E. S., Soares, F. P., de Abreu, E. V., et al. (2023). Systematic review of Platelet-Rich Plasma for low back pain. Biomedicines, 11(9), 2404.
Wongjarupong, A., Pairuchvej, S., Laohapornsvan, P., Kotheeranurak, V., Jitpakdee, K., Yeekian, C., & Chanplakorn, P. (2023). Platelet-Rich Plasma epidural injection an emerging strategy in lumbar disc herniation: A randomized controlled trial. BMC Musculoskeletal Disorders, 24, 335.
Saraf, A., Hussain, A., Sandhu, A. S., Bishnoi, S., & Arora, V. (2023). Transforaminal injections of Platelet-Rich Plasma compared with steroid in lumbar radiculopathy: A prospective, double-blind randomized study. Indian Journal of Orthopaedics, 57(7), 1126-1133.
Gupta, A., Chhabra, H. S., Singh, V., & Nagarjuna, D. (2024). Lumbar transforaminal injection of steroids versus Platelet-Rich Plasma for prolapse lumbar intervertebral disc with radiculopathy: A randomized double-blind controlled pilot study. Asian Spine Journal, 18(1), 58-65.
Wang, S., Liu, Z., Wang, J., et al. (2024). Platelet-Rich Plasma in nerve repair. Regenerative Therapy, 27, 244-250.
Shang, K., Liu, Y., et al. (2025). Platelet-Rich Plasma in peripheral nerve injury repair: A comprehensive review of mechanisms, clinical applications, and therapeutic potential. Experimental Biology and Medicine, 250, 10746.
Jimenez, A. (n.d.). Why choose our clinical team?. DrAlexJimenez.com.
Jimenez, A. (n.d.). Telemedicine sciatica relief with Dr. Jimenez. DrAlexJimenez.com.
NHS. (n.d.). Sciatica. NHS.
Cleveland Clinic. (2024). Cauda equina syndrome: What it is, symptoms and treatment. Cleveland Clinic.
Jimenez, A. (n.d.). Dr. Alexander Jimenez DC, APRN, FNP-BC, IFMCP, CFMP, ATN. LinkedIn.
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


Comments are closed.