Table of Contents
Introduction
As everyone knows, the gut helps the body metabolize nutrients and vitamins that it needs to function correctly. The gut system also allows the body’s immunity to perform while staying in communication with the brain. The gut helps sends signals back and forth to regulate the body’s hormones signals and other beneficial substances that the body requires. The gut is also in communication with the largest organ in the body, which is the skin. When intolerable factors start to wreck the gut and cause chaos inside the gut system, it disrupts the brain signals in the nervous system and can also take a toll on the skin. Today’s article will focus on a skin condition known as rosacea, how it affects the gut system, and what is the gut-skin connection. Referring patients to certified, skilled providers who specialize in gastroenterology treatments. We provide guidance to our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is critical for asking insightful questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.
What Is Rosacea?
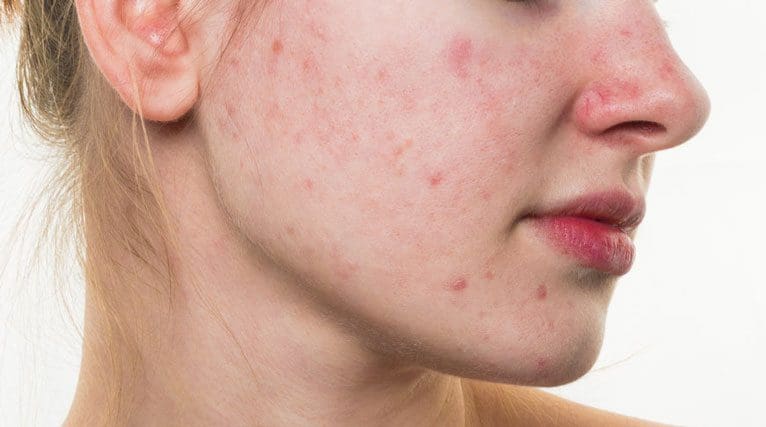
Have you felt any gut disorders like IBS, leaky gut, or GERD affecting your mid-section? How about redness around your face, especially the nose and cheek areas? Does your skin seem to feel tender to the touch in certain areas? Most of these symptoms are related to a chronic inflammatory disease known as rosacea. It is usually indicated by genetic and environmental components that can trigger rosacea initiation on the skin. Rosacea is generally aggravated by dysregulation of the body’s innate and adaptive immune system. Research studies have mentioned that rosacea is usually developed by lymphatic dilation and blood vessels exposed to extreme temperatures, spices, or alcohol which causes rosacea to affect the cheeks and nose. Not only that, but genetics, immune reaction, microorganisms, and environmental factors lead to various mediators such as keratinocytes, endothelial cells, mast cells, macrophages, T helper type 1 (TH1), and TH17 cells.
How Does It Affect The Gut System?
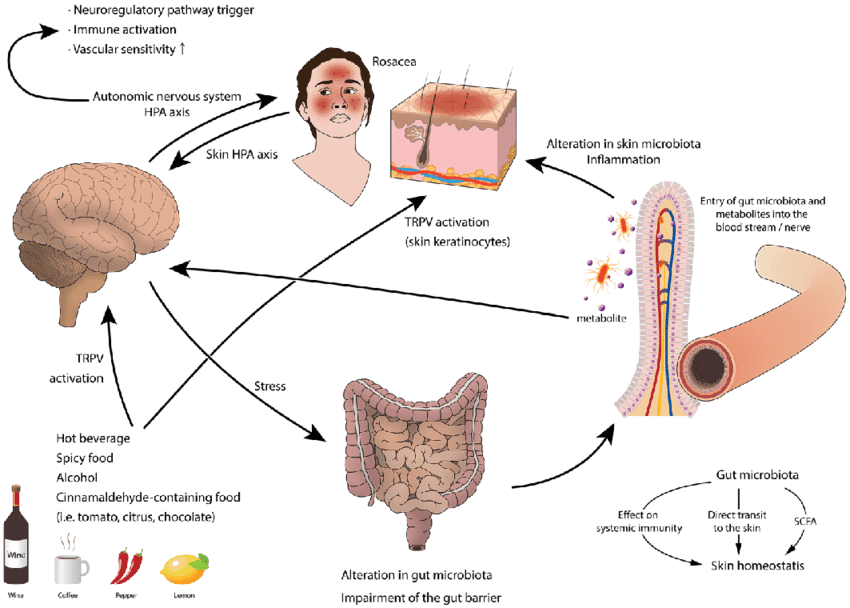
Since rosacea is developed through exposure to high temperatures, spices, or alcohol, research studies have shown that particular food and drinks cause the inflammatory cytokines to become triggered in the face. Additionally, many trigger factors can directly communicate to the cutaneous nervous system; neurovascular and neuro-immune active neuropeptides are lead to the manifestation of rosacea lesions. Some of the other triggers that can cause rosacea to develop is an unhealthy gut system. A study showed that more than 50% had low stomach acid among patients who had both rosacea and dyspepsia. The bacteria H.pylori resides in the stomach and has been recognized to trigger inflammation and gastrin-induced flushing, thus causing rosacea. Additional studies have mentioned that rosacea individuals will experience some gut disorders to occur. Since the gut system can succumb to various factors, it can affect the gut’s composition and trigger rosacea. Since the gut microbiota has influenced the body’s homeostasis, it can also influence the skin. When there are factors that trigger the intestinal barrier of the gut, it can affect the skin, causing the inflammatory cytokines to proceed with the development of rosacea.
Uncovering The Gut-Skin Connection-Video
Does your skin feel flushed due to extreme temperatures or consuming spicy food? Have you experienced gut disorders like SIBO, GERD, or leaky gut? Has your skin seemed to break out even more than it should? Your skin could be affected by your gut microbiota, as the video above shows what the gut-skin connection is and how they work with each other. Research studies have shown that since the gut microbiome is the key regulator of the body’s immune system, it plays a vital role in various skin disorders. This means that when environmental factors affect the gut’s microbiome, it also affects the skin through dysbiosis.
What Is The Gut-Skin Connection?
As stated earlier, the gut system is home to trillions of microorganisms that help metabolize the body’s homeostasis, including the largest organ, the skin. Research studies have found that when the gut microbial and the skin communicate with each other. It creates a bidirectional connection. The gut microbiome is also an essential mediator of inflammation in the gut and affects the skin. When there are factors like insulin resistance, imbalances in the sex hormones, gut inflammation, and microbial dysbiosis wrecking the gut system, the effects can cause the pathology of many inflammatory disorders to affect the skin. Any changes to the gut can also affect the skin as the gut consumes food to be biotransformed into nutrients that the body needs. But when food allergies and sensitivities affect the gut, the skin also gets involved, causing skin disorders like rosacea.
Conclusion
Overall the gut makes sure that the body is functioning correctly by metabolizing nutrients from consumed foods. The gut system has a connection to not only the brain and immune system but also the skin. The gut-skin connection goes hand in hand as factors that affect the gut can also affect the skin in developing skin disorders like rosacea. When a person is suffering from gut disorders, their skin is also damaged by factors like stress, food sensitivities, and skin disorders that can become a nuisance. This can be alleviated through small changes like reducing stress, eating healthy foods, and exercising, which are beneficial for relieving gut and skin disorders for individuals who want to get their health back.
References
Daou, Hala, et al. “Rosacea and the Microbiome: A Systematic Review.” Dermatology and Therapy, Springer Healthcare, Feb. 2021, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7859152/.
De Pessemier, Britta, et al. “Gut-Skin Axis: Current Knowledge of the Interrelationship between Microbial Dysbiosis and Skin Conditions.” Microorganisms, MDPI, 11 Feb. 2021, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7916842/.
Farshchian, Mehdi, and Steven Daveluy. “Rosacea.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 30 Dec. 2021, https://www.ncbi.nlm.nih.gov/books/NBK557574/.
Kim, Hei Sung. “Microbiota in Rosacea.” American Journal of Clinical Dermatology, Springer International Publishing, Sept. 2020, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7584533/.
Mikkelsen, Carsten Sauer, et al. “Rosacea: A Clinical Review.” Dermatology Reports, PAGEPress Publications, Pavia, Italy, 23 June 2016, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5134688/.
Salem, Iman, et al. “The Gut Microbiome as a Major Regulator of the Gut-Skin Axis.” Frontiers in Microbiology, Frontiers Media S.A., 10 July 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6048199/.
Disclaimer
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



Comments are closed.