From time to time, children and adolescents hear from those who care for them that they should “sit up straight” or “stand tall.”
Generally, these suggestions simply ask for an adjustment in posture. However, a change in stance, uneven shoulder height or a perceived inability to maintain a level hemline of the skirt of an adolescent girl may indicate a true spine deformity.
Scoliosis, or a sideways curve of the spine, is a condition that occurs in otherwise healthy children and adolescents, often with few if any symptoms.
Some degree of scoliosis is relatively common. Very small curves may be detected in as many as two to three out of 100 people.
As scoliosis is related to growth, the curve may be quite small in younger-aged children, and therefore not readily apparent. The curvature becomes a concern as the severity increases with growth of the child.
Although scoliosis can occur at any age, most curves become more obvious during the adolescent growth spurt. Small curves occur with similar frequency in boys and girls, but girls are more likely to progress to the point of requiring treatment.
Diagnosis
The underlying cause of scoliosis may sometimes be related to a defect in bone development or other conditions such as cerebral palsy or muscular dystrophy. However, the vast majority of cases are seen in healthy, active adolescents.
Scoliosis can run in families, but the exact cause of most cases is not known.
Scoliosis does not usually cause any pain. Your child’s primary care physician should inquire about your child’s strength and activity, as the evaluation of scoliosis requires a thorough medical history to determine if any other problems may be causing the spine to curve.
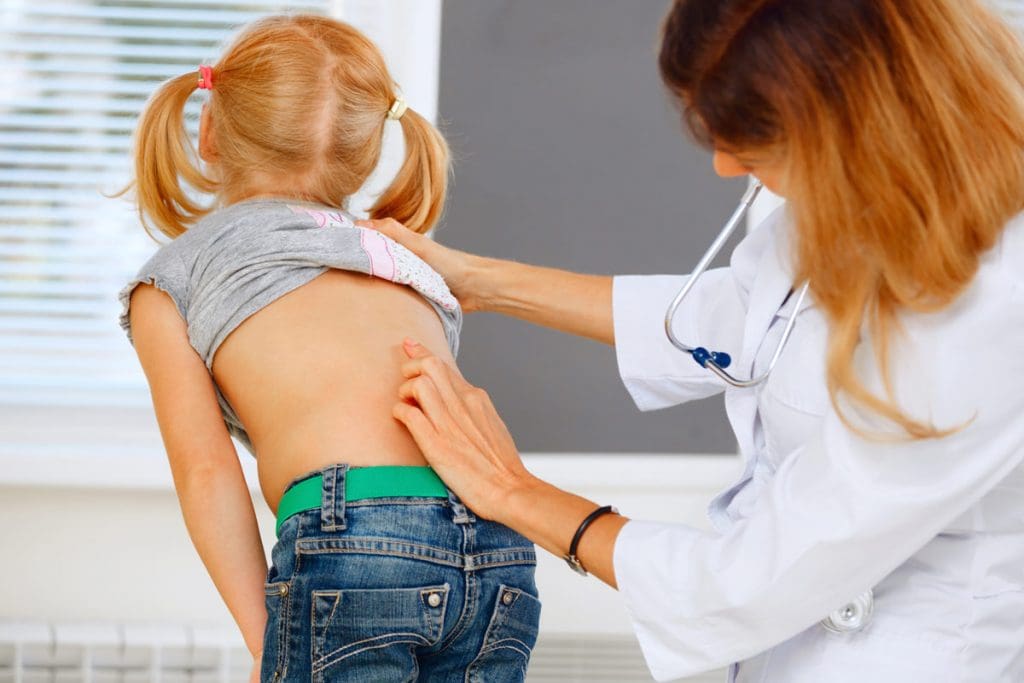
During an examination, the doctor will ask your child to bend forward, which will highlight any deformities. The nature and severity of the spine deformities are determined with an x-ray of the spine. The type of treatment required depends on:
- The kind of scoliosis
- The degree of the curve
- The number of remaining years of growth until the child reaches skeletal maturity
The main categories of scoliosis in children and adolescents are as follows:
- Adolescent idiopathic scoliosis – By far the most common type of scoliosis; occurs after the age of 10 and may progress quickly during the adolescent growth spurt. The exact cause in idiopathic scoliosis is unknown.
- Juvenile idiopathic scoliosis – Occurs in children between the ages of 3 and 10 years and is uncommon. Although the curves progress slowly, as children of this age do not grow quickly, their young age may allow considerable time for the curves to progress before the child reaches maturity.
- Early onset or infantile scoliosis – Occurs in children younger than 3 and may progress to an extreme severity, interfering with growth and breathing.
Treatment
Treatment options are limited to observation, casting/bracing or surgery. Physical therapy, chiropractic care and electrical stimulation of the muscles of the back have not been shown to change the curve nor alter its risk of progression. Severe deformities and those at risk to progress to unacceptable deformity or to the point of interfering in function warrant treatment.
Source:
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card


Comments are closed.