Dietary Strategies:
Abstract: Metabolic syndrome (MetS) is established as the combination of central obesity and different metabolic disturbances, such as insulin resistance, hypertension and dyslipidemia. This cluster of factors affects approximately 10%–50% of adults worldwide and the prevalence has been increasing in epidemic proportions over the last years. Thus, dietary strategies to treat this heterogenic disease are under continuous study. In this sense, diets based on negative-energy-balance, the Mediterranean dietary pattern, n-3 fatty acids, total antioxidant capacity and meal frequency have been suggested as effective approaches to treat MetS. Furthermore, the type and percentage of carbohydrates, the glycemic index or glycemic load, and dietary fiber content are some of the most relevant aspects related to insulin resistance and impaired glucose tolerance, which are important co-morbidities of MetS. Finally, new studies focused on the molecular action of specific nutritional bioactive compounds with positive effects on the MetS are currently an objective of scientific research worldwide. The present review summarizes some of the most relevant dietary approaches and bioactive compounds employed in the treatment of the MetS to date.
Keywords: metabolic syndrome; dietary strategies; bioactive compounds
Table of Contents
1. Metabolic Syndrome
 It was during the period between 1910 and 1920 when it was suggested for the first time that a cluster of associated metabolic disturbances tended to coexist together [1]. Since then, different health organisms have suggested diverse definitions for metabolic syndrome (MetS) but there has not yet been a well-established consensus. The most common definitions are summarized in Table 1. What is clear for all of these is that the MetS is a clinical entity of substantial heterogeneity, commonly represented by the combination of obesity (especially abdominal obesity), hyperglycemia, dyslipidemia and/or hypertension [2–6].
It was during the period between 1910 and 1920 when it was suggested for the first time that a cluster of associated metabolic disturbances tended to coexist together [1]. Since then, different health organisms have suggested diverse definitions for metabolic syndrome (MetS) but there has not yet been a well-established consensus. The most common definitions are summarized in Table 1. What is clear for all of these is that the MetS is a clinical entity of substantial heterogeneity, commonly represented by the combination of obesity (especially abdominal obesity), hyperglycemia, dyslipidemia and/or hypertension [2–6].

Obesity consists of an abnormal or excessive fat accumulation, for which the main cause is a chronic imbalance between energy intake and energy expenditure [7,8]. The excess of energy consumed is primarily deposited in the adipose tissue as triglycerides (TG) [9].
Dyslipidemia encompasses elevated serum TG levels, increased low density lipoprotein- cholesterol (LDL-c) particles, and reduced levels of high density lipoprotein-cholesterol (HDL-c) [10]. It is associated with hepatic steatosis [11], dysfunction of pancreatic β-cells [12] and elevated risk of atherosclerosis [13], among others.
Another main modifiable MetS manifestation is hypertension, which is mainly defined as a resting systolic blood pressure (SBP) ≥ 140 mmHg or diastolic blood pressure (DBP) ≥ 90 mmHg or drug prescription to lower hypertension [14]. It usually involves narrowed arteries and is identified as a major cardiovascular and renal risk factor, related to heart and vascular disease, stroke and myocardial infarction [13,15–17].
Hyperglycemia, related insulin resistance and type 2 diabetes mellitus are characterized by an impaired uptake of glucose by the cells, that lead to elevated plasma glucose levels, glycosuria and ketoacidosis [18]. It is responsible for different tissue damage that shortens the life expectancy of diabetics, involving cardiovascular diseases (CVD), atherosclerosis, hypertension [19], β-cell dysfunction [12], kidney disease [20] or blindness [21]. Currently, diabetes is considered the leading cause of death in developed countries [22].
Moreover, oxidative stress and low grade inflammation are two important mechanisms implicated in the etiology, pathogenesis, and development of MetS [23]. Oxidative stress is defined as an imbalance between the pro-oxidants and antioxidants in the body [24]. It plays a key role in the development of atherosclerosis by different mechanisms such as the oxidation of LDL-c particles [25] or impairment of HDL-c functions [26]. Inflammation is an immune system response to injury hypothesized to be a major mechanism in the pathogenesis and progression of obesity related disorders and the link between adiposity, insulin resistance, MetS and CVD [27].
Although the prevalence of the MetS varies broadly around the word and depends on the source used for its definition, it is clear that over the last 40–50 years the number of people presenting with this syndrome has risen in epidemic proportions [28]. Moreover, the frequency of this syndrome is increased in developed countries, sedentary people, smokers, low socioeconomic status population, as well as in individuals with unhealthy dietary habits [29,30].
For all of this, there is currently a wide concern to find effective strategies to detect, treat and control the comorbidities associated with MetS. This is a complex challenge as MetS is a clinical entity of substantial heterogeneity and therefore, the different cornerstones implicated in its development should be addressed. In this review we compiled and examined different dietary patterns and bioactive compounds that have pointed out to be effective in MetS treatment.
2. Dietary Patterns
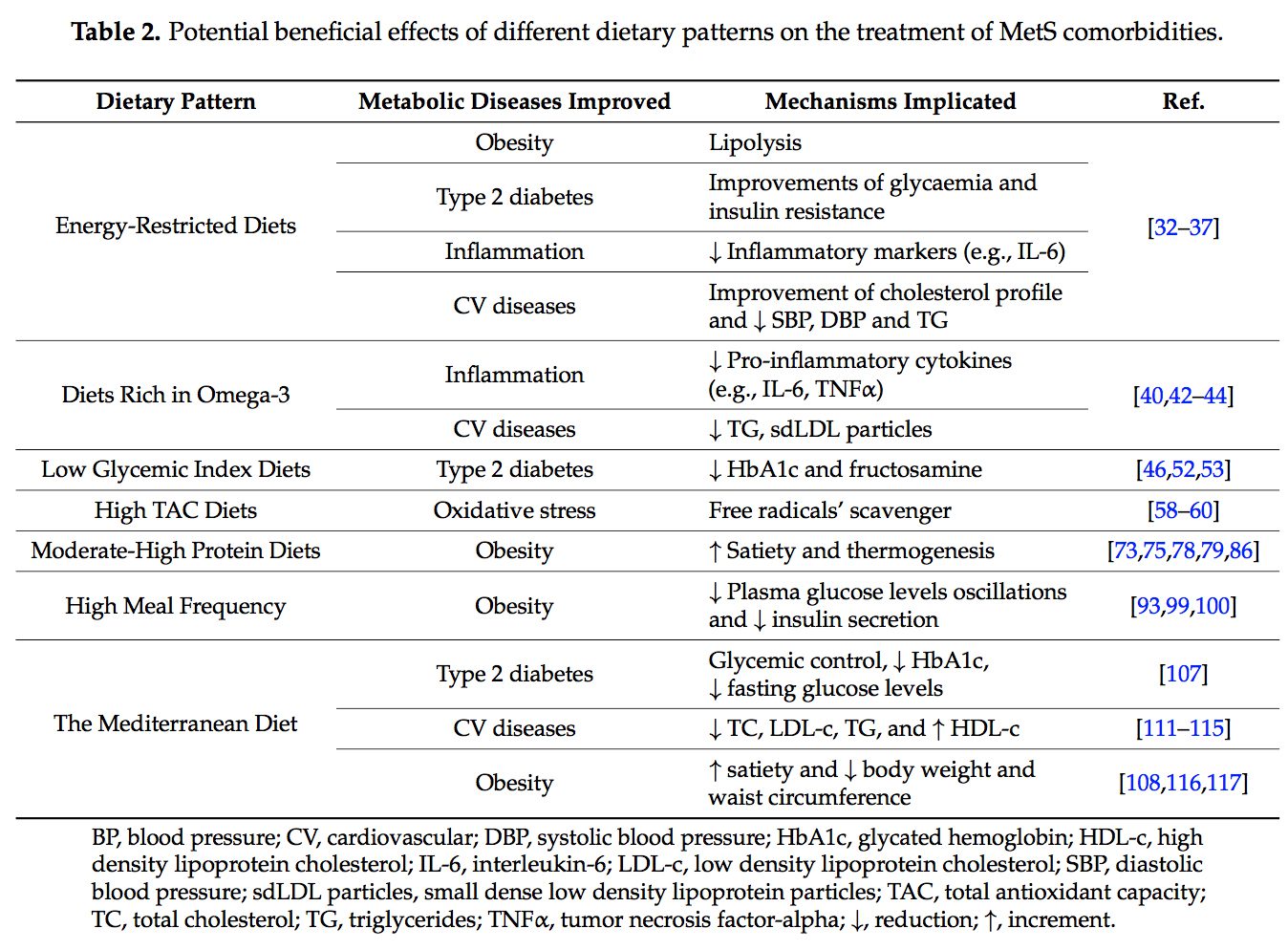
 Several dietary strategies and their potential positive effects on the prevention and treatment of the different metabolic complications associated to the MetS, are described below and summarized in Table 2.
Several dietary strategies and their potential positive effects on the prevention and treatment of the different metabolic complications associated to the MetS, are described below and summarized in Table 2.
 2.1. Energy-Restricted Diet Strategies
2.1. Energy-Restricted Diet Strategies

Energy restricted diets are probably the most commonly used and studied dietary strategies for combating excess weight and related comorbidities. They consist in personalized regimes that supply less calories than the total energy expended by a specific individual [31].
A hypocaloric diet results in a negative energy balance and subsequently, in body weight reduction [31]. Weight loss is achieved via fat mobilization from different body compartments as a consequence of the lipolysis process necessary to provide energy substrate [32,33]. In people who are overweight or suffering from obesity, as is the case of most people with MetS, weight loss is important as it is associated with improvement of related disorders such as abdominal obesity (visceral adipose tissue), type 2 diabetes, CVD or inflammation [32–36].
Moreover, as described above, low grade inflammation is associated with MetS and obesity. Therefore, of particular importance is the fact that in obese individuals following a hypocaloric diet, a depletion of plasma inflammatory markers such as interleukin (IL)-6 has been observed [34]. Thus, caloric restriction in obese people suffering MetS may improve the whole-body pro-inflammatory state.
At the same time, body weight reduction is associated with improvements in cellular insulin signal transduction, increments in peripheral insulin sensitivity and higher robustness in insulin secretory responses [32,36]. People with excess body weight who are at risk of developing type 2 diabetes, may benefit from a hypocaloric regime by improving plasma glucose levels and insulin resistance.
In addition, different intervention trials have reported a relationship between energy restricted diets and lower risk of developing CVD. In this sense, in studies with obese people following a hypocaloric diet, improvements in lipid profile variables such as reductions of LDL-c and plasma TG levels, as well as improvements in hypertension via depletion of SBP and DBP levels have been observed [35,37].
Among the different nutritional intervention trials, a reduction of 500–600 kcal a day of the energy requirements is a well-established hypocaloric dietary strategy, which has demonstrated to be effective in weight reduction [38,39]. However, the challenge lies in maintaining the weight loss over time, as many subjects can follow a prescribed diet for a few months, but most people have difficulty in maintaining the acquired habits over the long term [40,41].
2.2. Diets Rich in Omega-3 Fatty Acids
 The very long-chain eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) are essential omega-3 polyunsaturated fatty acids (n-3 PUFAs) for human physiology. Their main dietary sources are fish and algal oils and fatty fish, but they can also be synthesized by humans from α-linolenic acid [40].
The very long-chain eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) are essential omega-3 polyunsaturated fatty acids (n-3 PUFAs) for human physiology. Their main dietary sources are fish and algal oils and fatty fish, but they can also be synthesized by humans from α-linolenic acid [40].
There is a moderate body of evidence suggesting that n-3 PUFAs, mainly EPA and DHA, have a positive role in the prevention and treatment of the pathologies associated to MetS [42].
In this context, it has been described that EPA and DHA have the ability to reduce the risk of developing CVD and cardiometabolic abnormalities as well as CVD-related mortality [42]. These beneficial effects are thought to be mainly due to the ability of these essential fatty acids to reduce plasma TG levels [43].
Moreover, different studies have shown that people following an increased n-3 PUFA diet have reduced plasma levels of the pro-inflammatory cytokines IL-6 and tumor necrosis factor-alpha (TNFα), as well as plasma C-reactive protein (CRP) [44]. These effects are probably mediated by resolvins, maresins and protectins, which are EPA and DHA metabolic products with anti-inflammatory properties [44].
There are some studies that have observed an association between n-3 ingestion and improvements or prevention of type 2 diabetes development. However, other studies found opposite results [44]. Thus, it cannot be made any specific affirmation in this respect.
The European Food Safety Authority recommends and intake of 250 mg EPA + DHA a day, in the general healthy population as a primary prevention of CVD [45]. These amounts can be achieved with an ingestion of 1–2 fatty fish meals per week [45].
2.3. Diets Based on Low Glycemic Index/Load
 Over the last ten years, the concern about the quality of the carbohydrates (CHO) consumed has risen [46]. In this context, the glycemic index (GI) is used as a CHO quality measure. It consists in a ranking on a scale from 0 to 100 that classifies carbohydrate-containing foods according to the postprandial glucose response [47]. The higher the index, the more promptly the postprandial serum glucose rises and the more rapid the insulin response. A quick insulin response leads to rapid hypoglycemia, which is suggested to be associated with an increment of the feeling of hunger and to a subsequent higher caloric intake [47]. The glycemic load (GL) is equal to the GI multiplied by the number of grams of CHO in a serving [48].
Over the last ten years, the concern about the quality of the carbohydrates (CHO) consumed has risen [46]. In this context, the glycemic index (GI) is used as a CHO quality measure. It consists in a ranking on a scale from 0 to 100 that classifies carbohydrate-containing foods according to the postprandial glucose response [47]. The higher the index, the more promptly the postprandial serum glucose rises and the more rapid the insulin response. A quick insulin response leads to rapid hypoglycemia, which is suggested to be associated with an increment of the feeling of hunger and to a subsequent higher caloric intake [47]. The glycemic load (GL) is equal to the GI multiplied by the number of grams of CHO in a serving [48].
There is a theory which states that MetS is a consequence of an elevated intake of high GI foods over time, among others unhealthy dietary habits [49]. In this sense, following a diet rich in high GI CHO has been associated with hyperglycemia, insulin resistance, type 2 diabetes, hypertriglyceridemia, CVD, and obesity [47,50,51], abnormalities directly related to MetS.
On the contrary, a low GI diet has been associated with slower absorption of the CHO and subsequently smaller blood glucose fluctuations, which indicate better glycemic control [46]. In patients with type 2 diabetes, diets based on low GI are associated with reductions in glycated hemoglobin (HbA1c) and fructosamine blood levels, two biomarkers used as key monitoring factors in diabetes management [52,53].
For all of this, it is common to find the limitation of CHO at high GI among the advice for MetS treatment [28], in particular with respect to “ready-to-eat processed foods” including sweetened beverages, soft drinks, cookies, cakes, candy, juice drinks, and other foods which contain high amounts of added sugars [54].
2.4. Diets with High Total Antioxidant Capacity
 Dietary total antioxidant capacity (TAC) is an indicator of diet quality defined as the sum of antioxidant activities of the pool of antioxidants present in a food [55]. These antioxidants have the capacity to act as scavengers of free radicals and other reactive species produced in the organisms [56]. Taking into account that oxidative stress is one of the remarkable unfortunate physiological states of MetS, dietary antioxidants are of main interest in the prevention and treatment of this multifactorial disorder [57]. Accordingly, it is well-accepted that diets with a high content of spices, herbs, fruits, vegetables, nuts and chocolate, are associated with a decreased risk of oxidative stress-related diseases development [58–60]. Moreover, several studies have analyzed the effects of dietary TAC in individuals suffering from MetS or related diseases [61,62]. In the Tehran Lipid and Glucose Study it was demonstrated that a high TAC has beneficial effects on metabolic disorders and especially prevents weight and abdominal fat gain [61]. In the same line, research conducted in our institutions also evidenced that beneficial effects on body weight, oxidative stress biomarkers and other MetS features were positively related with higher TAC consumption in patients suffering from MetS [63–65].
Dietary total antioxidant capacity (TAC) is an indicator of diet quality defined as the sum of antioxidant activities of the pool of antioxidants present in a food [55]. These antioxidants have the capacity to act as scavengers of free radicals and other reactive species produced in the organisms [56]. Taking into account that oxidative stress is one of the remarkable unfortunate physiological states of MetS, dietary antioxidants are of main interest in the prevention and treatment of this multifactorial disorder [57]. Accordingly, it is well-accepted that diets with a high content of spices, herbs, fruits, vegetables, nuts and chocolate, are associated with a decreased risk of oxidative stress-related diseases development [58–60]. Moreover, several studies have analyzed the effects of dietary TAC in individuals suffering from MetS or related diseases [61,62]. In the Tehran Lipid and Glucose Study it was demonstrated that a high TAC has beneficial effects on metabolic disorders and especially prevents weight and abdominal fat gain [61]. In the same line, research conducted in our institutions also evidenced that beneficial effects on body weight, oxidative stress biomarkers and other MetS features were positively related with higher TAC consumption in patients suffering from MetS [63–65].
In this sense, the World Health Organization (WHO) recommendation for fruit and vegetables consumption (high TAC foods) for the general population is a minimum of 400 g a day [66]. Moreover, cooking with spices is recommended in order to increase the TAC dietary intake and, at the same time, maintain flavor while reducing salt [67].
2.5. Moderate-High Protein Diets
 The macronutrient distribution set in a weight loss dietary plan has commonly been 50%–55% total caloric value from CHO, 15% from proteins and 30% from lipids [57,68]. However, as most people have difficulty in maintaining weight loss achievements over time [69,70], research on increment of protein intake (>20%) at the expense of CHO was carried out [71–77].
The macronutrient distribution set in a weight loss dietary plan has commonly been 50%–55% total caloric value from CHO, 15% from proteins and 30% from lipids [57,68]. However, as most people have difficulty in maintaining weight loss achievements over time [69,70], research on increment of protein intake (>20%) at the expense of CHO was carried out [71–77].
Two mechanisms have been proposed to explain the potential beneficial effects of high-moderate protein diets: the increment of diet-induced thermogenesis [73] and the increase of satiety [78]. The increment of the thermogenesis is explained by the synthesis of peptide bonds, production of urea and gluconeogenesis, which are processes with a higher energy requirement than the metabolism of lipids or CHO [75]. An increment of different appetite-control hormones such as insulin, cholecystokinin or glucagon-like peptide 1, may clarify the satiety effect [79].
Other beneficial effects attributed to moderate-high protein diets in the literature are the improvement of glucose homeostasis [80], the possibility of lower blood lipids [81], the reduction of blood pressure [82], the preservation of lean body mass [83] or the lower of cardiometabolic disease risk [84,85]. However, there are other studies that have not found benefits associated to a moderate-high protein diet [76]. This fact may be explained by the different type of proteins and their amino acid composition [80], as well as by the different type of populations included in each study [85]. Therefore, more research in the field is needed in order to make these results consistent.
In any case, when a hypocaloric diet is implemented, it is necessary to slightly increase the amount of proteins. Otherwise it would be difficult to reach the protein energy requirements, established as 0.83 g/kg/day for isocaloric diets and which should probably be at least 1 g/kg/day for energy-restricted diets [86].
2.6. High Meal Frequency Pattern

The pattern of increasing meal frequency in weight loss and weight control interventions has currently become popular among professionals [87,88]. The idea is to distribute the total daily energy intake into more frequently and smaller meals. However, there is no strong evidence about the efficacy of this habit yet [89]. While some investigations have found an inverse association between the increment of meals per day and body weight, body mass index (BMI), fat mass percentage or metabolic diseases such as coronary heart disease or type 2 diabetes [71,88,90–92], others have found no association [93–95].
Different mechanisms by which high meal frequency can have a positive effect on weight and metabolism management have been proposed. An increment of energy expenditure was hypothesized; however, the studies carried out in this line have concluded that total energy expenditure does not differ among different meal frequencies [96,97]. Another postulated hypothesis is that the greater the number of meals a day, the higher the fat oxidation, but again no consensus has been achieved [89,98]. An additional suggested mechanism is that increasing meal frequency leads to plasma glucose levels with lower oscillations and reduced insulin secretion which is thought to contribute to a better appetite control. However, these associations have been found in population with overweight or high glucose levels but in normal-weight or normoglycaemic individuals the results are still inconsistent [93,99–101].
2.7. The Mediterranean Diet
 The concept of the Mediterranean Diet (MedDiet) was for the first time defined by the scientific Ancel Keys who observed that those countries around the Mediterranean Sea, which had a characteristic diet, had less risk of suffering coronary heart diseases [102,103].
The concept of the Mediterranean Diet (MedDiet) was for the first time defined by the scientific Ancel Keys who observed that those countries around the Mediterranean Sea, which had a characteristic diet, had less risk of suffering coronary heart diseases [102,103].
The traditional MedDiet is characterized by a high intake of extra-virgin olive oil and plant foods (fruits, vegetables, cereals, whole grains, legumes, tree nuts, seeds and olives), low intakes of sweets and red meat and moderate consumption of dairy products, fish and red wine [104].
There is a lot of literature supporting the general health benefits of the MedDiet. In this sense, it has been reported that a high adherence to this dietary pattern protects against mortality and morbidity from several causes [105]. Thus, different studies suggested the MedDiet as a successful tool for the prevention and treatment of MetS and related comorbidities [106–108]. Moreover, recent meta-analysis concluded that the MedDiet is associated with less risk of developing type 2 diabetes and with a better glycemic control in people with this metabolic disorder [107,109,110]. Other studies have found a positive correlation between the adherence to a MedDiet pattern and reduced risk of developing CVD [111–114]. In fact, many studies have found a positive association between following a MedDiet and improvements in lipid profile by reduction of total cholesterol, LDL-c and TG, and an increase in HDL-c [111–115]. Finally, different studies also suggest that the MedDiet pattern may be a good strategy for obesity treatment as it has been associated with significant reductions in body weight and waist circumference [108,116,117].
The high amount of fiber which, among other beneficial effects, helps to weight control providing satiety; and the high antioxidants and anti-inflammatory nutrients such as n-3 fatty acids, oleic acid or phenolic compounds, are thought to be the main contributors to the positive effects attributed to the MedDiet [118].
For all these reasons, efforts to maintain the MedDiet pattern in Mediterranean countries and to implement this dietary habits in westernized countries with unhealthy nutritional patterns should be made.
3. Dietary: Single Nutrients and Bioactive Compounds
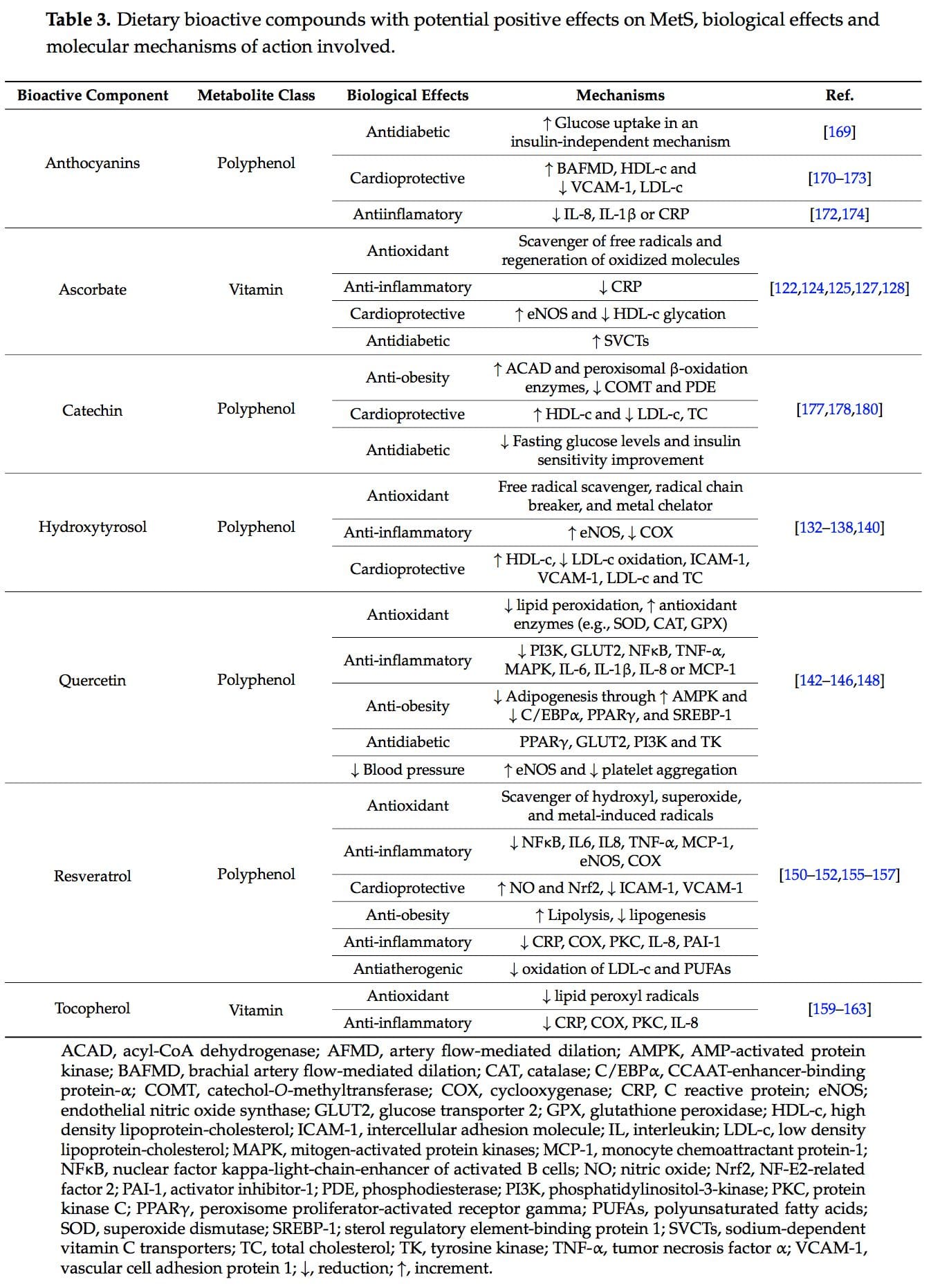
 New studies focused on the molecular action of nutritional bioactive compounds with positive effects on MetS are currently an objective of scientific research worldwide with the aim of designing more personalized strategies in the framework of molecular nutrition. Among them, flavonoids and antioxidant vitamins are some of the most studied compounds with different potential benefits such as antioxidant, vasodilatory, anti-atherogenic, antithrombotic, and anti-inflammatory effects [119]. Table 3 summarizes different nutritional bioactive compounds with potential positive effects on MetS, including the possible molecular mechanism of action involved.
New studies focused on the molecular action of nutritional bioactive compounds with positive effects on MetS are currently an objective of scientific research worldwide with the aim of designing more personalized strategies in the framework of molecular nutrition. Among them, flavonoids and antioxidant vitamins are some of the most studied compounds with different potential benefits such as antioxidant, vasodilatory, anti-atherogenic, antithrombotic, and anti-inflammatory effects [119]. Table 3 summarizes different nutritional bioactive compounds with potential positive effects on MetS, including the possible molecular mechanism of action involved.
3.1. Ascorbate
 Vitamin C, ascorbic acid or ascorbate is an essential nutrient as human beings cannot synthesize it. It is a water-soluble antioxidant mainly found in fruits, especially citrus (lemon, orange), and vegetables (pepper, kale) [120]. Several beneficial effects have been associated to this vitamin such as antioxidant and anti-inflammatory properties and prevention or treatment of CVD and type 2 diabetes [121–123].
Vitamin C, ascorbic acid or ascorbate is an essential nutrient as human beings cannot synthesize it. It is a water-soluble antioxidant mainly found in fruits, especially citrus (lemon, orange), and vegetables (pepper, kale) [120]. Several beneficial effects have been associated to this vitamin such as antioxidant and anti-inflammatory properties and prevention or treatment of CVD and type 2 diabetes [121–123].
This dietary component produces its antioxidant effect primarily by quenching damaging free radicals and other reactive oxygen and nitrogen species and therefore preventing molecules such as LDL-c from oxidation [122]. It can also regenerate other oxidized antioxidants like tocopherol [124].
Moreover, it has been described that ascorbic acid may reduce inflammation as it is associated with depletion of CRP levels [125]. This is an important outcome to take in consideration in the treatment of MetS sufferers, as they usually present low grade inflammation [27].
Supplementation with vitamin C have also been associated with prevention of CVD by improving the endothelial function [126] and probably by lowering blood pressure [121]. These effects are thought to be exerted by the ability of vitamin C to enhance the endothelial nitric oxide synthase enzyme (eNOS) activity and to reduce HDL-c glycation [127].
Additionally, several studies have attributed to ascorbate supplementation an antidiabetic effect by improving whole body insulin sensitivity and glucose control in people with type 2 diabetes [123]. These antidiabetic properties are thought to be mediated by optimization of the insulin secretory function of the pancreatic islet cells by increasing muscle sodium-dependent vitamin C transporters (SVCTs) [128].
Despite all of this, it should be taken into account that most people reach ascorbic acid requirements (established at 95–110 mg/day in the general population) from diet and do not need supplementation [122,129]. Besides, it should be considered that an excess of vitamin C ingestion leads to the opposite effect and oxidative particles are formed [130,131].
3.2. Hydroxytyrosol
 Hydroxytyrosol (3,4-dihydroxyphenylethanol) is a phenolic compound mainly found in olives [132].
Hydroxytyrosol (3,4-dihydroxyphenylethanol) is a phenolic compound mainly found in olives [132].
It is considered the strongest antioxidant of olive oil and one of the main antioxidants in nature [133]. It acts as a powerful scavenger of free radicals, as a radical chain breaker and as metal chelator [134]. It has the ability of inhibiting LDL-c oxidation by macrophages [132]. In this sense, it is the only phenol recognized by the European Food Safety Authority (EFSA) as a protector of blood lipids from oxidative damage [135].
Hydroxytyrosol has also been reported to have anti-inflammatory effects, probably by suppressing cyclooxygenase activity and inducing eNOS expression [136]. Thus, enhancement of olives/olive oil intakes or hydroxytyroxol supplementation in people suffering from MetS may be a good strategy in order to improve inflammatory status.
Another beneficial effect attributed to this phenolic compound is its cardiovascular protective effect. It presents anti-atherogenic properties by decreasing the expression of vascular cell adhesion protein 1 (VCAM-1) and intercellular adhesion molecule 1 (ICAM-1) [132,137], which are probably the result of an inactivation of the nuclear factor kappa-light-chain-enhancer of activated B cells (NFκB), activator protein 1 (AP-1), GATA transcription factor and nicotinamide adenine dinucleotide phosphate (NAD(P)H) oxidase [138,139]. Hydroxytyrosol also provides antidyslipidemic effects by lowering plasma levels of LDL-c, total cholesterol and TG, and by rising HDL-c [138].
Despite the beneficial effects attributed to hydfroxytyrosol as an antioxidant, for its antiinflamatory properties and as cardiovascular protector, it should be taken into account that most studies focused on this compound have been performed with mixtures of olive phenols, thus a synergic effect cannot be excluded [140].
3.3. Quercetin
 Quercetin is a predominant flavanol naturally present in vegetables, fruits, green tea or red wine. It is commonly found as glycoside forms, where rutin is the most common and important structure found in nature [141].
Quercetin is a predominant flavanol naturally present in vegetables, fruits, green tea or red wine. It is commonly found as glycoside forms, where rutin is the most common and important structure found in nature [141].
Many beneficial effects that can contribute to MetS improvement have been attributed to quercetin. Among them, its antioxidant capacity should be highlighted, as it has been reported to inhibit lipid peroxidation and increase antioxidant enzymes such as superoxide dismutase (SOD), catalase (CAT) or glutathione peroxidase (GPX) [142].
Moreover, an anti-inflammatory effect mediated via attenuation of tumor necrosis factor α (TNF-α), NFκB and mitogen-activated protein kinases (MAPK), as well as depletion of IL-6, IL-1β, IL-8 or monocyte chemoattractant protein-1 (MCP-1) gene expression has also been attributed to this polyphenol [143].
As most people with MetS are overweight or obese, the role of quercetin in body weight reduction and obesity prevention has been of special interest. In this sense, it stands out the capacity of quercetin to inhibit adipogenesis through inducing the activation of AMP-activated protein kinase (AMPK) and decreasing the expression of CCAAT-enhancer-binding protein-α (C/EBPα), peroxisome proliferator-activated receptor gamma (PPARγ), and sterol regulatory element-binding protein 1 (SREBP-1) [141,144].
According to the antidiabetic effects, it is proposed that quercetin may act as an agonist of peroxisome proliferator-activated receptor gamma (PPARγ), and thus improve insulin-stimulated glucose uptake in mature adipocytes [145]. Moreover, quercetin may ameliorate hyperglycemia by inhibiting glucose transporter 2 (GLUT2) and insulin dependent phosphatidylinositol-3-kinase (PI3K) and blocking tyrosine kinase (TK) [142].
Finally, different studies observed that quercetin has the ability to reduce blood pressure [146–148]. However, the mechanisms of action are not clear, since some authors have suggested that quercetin increases eNOS, contributing to inhibition of platelet aggregation and improvement of the endothelial function [146,147], but there are other studies that have not come across these results [148].
3.4. Resveratrol

Resveratrol (3,5,4′-trihidroxiestilben) is a phenolic compound mainly found in red grapes and derived products (red wine, grape juice) [149]. It has shown antioxidant and anti-inflammatory activities, and cardioprotective, anti-obesity and antidiabetic capacities [150–156].
The antioxidant effects of resveratrol have been reported to be carried out by scavenging of hydroxyl, superoxide, and metal-induced radicals as well as by antioxidant effects in cells producing reactive oxygen species (ROS) [150].
Moreover, it has been reported that the anti-inflammatory effects of resveratrol are mediated by inhibiting NFκB signaling [151]. Furthermore, this polyphenol reduces the expression of proinflammatory cytokines such as interleukin 6 (IL-6), interleukin 8 (IL-8), TNF-α, monocyte chemoattractant protein-1 (MCP-1) and eNOS [152]. In addition, resveratrol inhibits the cyclooxygenase (COX) expression and activity, a pathway involved in the synthesis of proinflammatory lipid mediators [152].
Concerning the effects of resveratrol against development of type 2 diabetes, it has been reported that treatment of diabetes patients with this polyphenol provides significant improvements in the status of multiple clinically relevant biomarkers such as fasting glucose levels, insulin concentrations or glycated hemoglobin and Homeostasis Model Assessment Insulin Resistance (HOMA-IR) [153,154].
Additionally, cardioprotective effects have been attributed to resveratrol. In this sense, it is suggested that resveratrol improves the endothelial function by producing nitric oxide (NO) through increasing the activity and expression of eNOS. This effect is thought to be conducted through activation of nicotinamide adenine dinucleotide-dependent deacetylase sirtuin-1 (Sirt 1) and 5′ AMP-activated protein kinase (AMPK) [155]. Besides, resveratrol exerts endothelial protection by stimulation of NF-E2-related factor 2 (Nrf2) [156] and decreasing the expression of adhesion prote
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



 2.1. Energy-Restricted Diet Strategies
2.1. Energy-Restricted Diet Strategies
Comments are closed.