The sheer magnitude of America’s prescription opioid abuse epidemic has evoked visceral responses and calls-to-action from public and private sectors. As longtime advocates of drug-free management of acute, subacute and chronic back, neck and neuro-musculoskeletal pain, the chiropractic profession is aligned with these important initiatives and committed to actively participate in solving the prescription opioid addiction crisis.As professionals dedicated to health and well-being, Doctors of Chiropractic (DCs) are educated, trained and positioned to deliver non-pharmacologic pain management and play a leading role in “America’s Opioid Exit Strategy.”
Data released by the Centers for Disease Control and Prevention (CDC) revealed that opioid deaths continued to surge in 2015, surpassing 30,000 for the first time in recent history. CDC Director Tom Frieden said,“The epidemic of deaths involving opioids continues to worsen. Prescription opioid misuse and use of heroin and illicitly manufactured fentanyl are intertwined and deeply troubling problems.”1
The human toll of prescription opioid use, abuse, dependence, overdose and poisoning have rightfully become a national public health concern. Along with the tragic loss of life, it is also creating a monumental burden on our health and related health care costs:
- Health care costs for opioid abusers are eight times higher than for nonabusers.2
- A new retrospective cohort study shows a 72 percent increase in hospitalizations related to opioid abuse/dependence from 2002 to 2012. Not surprisingly, inpatient charges more than quadrupled over that time. Previous estimates of the annual excess costs of opioid abuse
to payers range from approximately $10,000 to $20,000 per patient, imposing a substantial economic burden on payers.3 - A recent government study puts the economic burden to the U.S. economy at $78.5 billion annually. For this study, CDC researchers analyzed the financial impact to include direct health care costs, lost productivity and costs to the criminal justice system.4
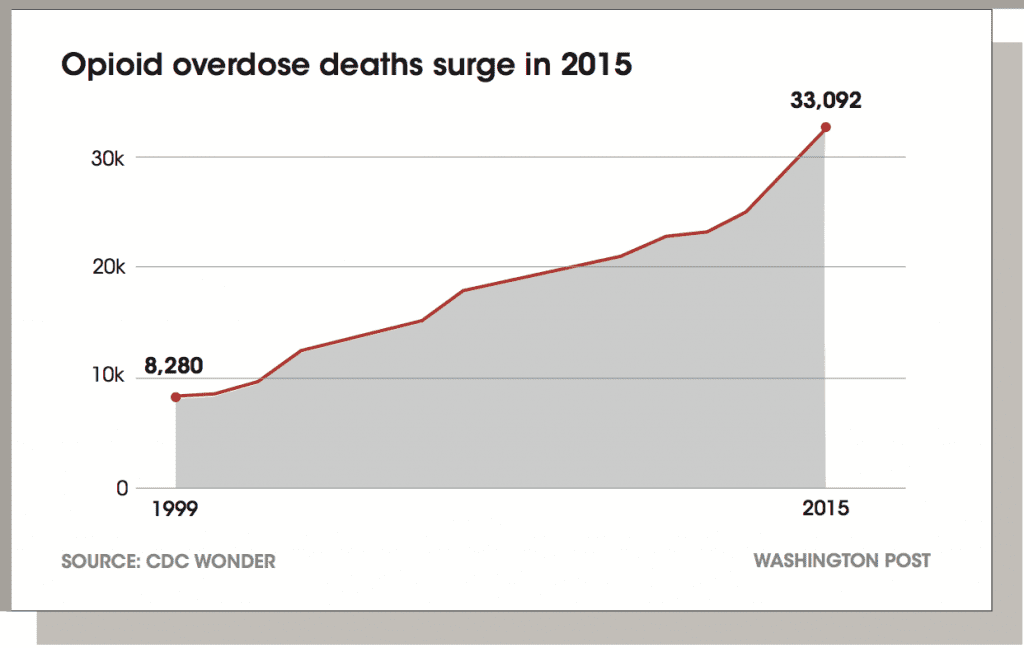
AMERICA’S COMMITMENT TO PRESCRIPTION OPIOID ABUSE: A PAINFUL REALITY CHECK
As a non-pharmacologic approach to effectively address acute, subacute and chronic non- cancer pain, integrative care management answers the needs of individuals nationwide.
With patient access to opioids becoming more restricted through more responsible clinician prescribing and government-mandated reduced production of opioids — and as those who are addicted become empowered to reduce their utilization — people experiencing pain face new, daunting challenges:
- Without the use of drugs, how will they cope with pain?
- How can they get referrals and access to drug-free care that will be effective for acute, subacute and chronic pain?
- How can they ensure that their health care plans and insurance will cover the cost of non- pharmacologic care?

While the chiropractic profession lauds many of the noteworthy announcements and strides to overcome opioid addiction, these recommendations fall short in providing meaningful answers and solutions for those who are suffering from pain.
It is encouraging to see the July 22, 2016 enactment of the Comprehensive Addiction and Recovery Act (P.L. 114-198), the first major federal addiction legislation in 40 years, and the most comprehensive effort undertaken to address the opioid epidemic. It encompasses all six pillars necessary for such a coordinated response – prevention, treatment, recovery, law enforcement, criminal justice reform and overdose reversal.5 The recent passage of the 21st Century Cures Act included $1 billion for states to use to fight opioid abuse.6 Unfortunately, this legislation has drawn critics who say it is simply a huge de-regulatory giveaway to the pharmaceutical and medical device industry.7
Closer examination of these legislative initiatives points to the absence of programs that address non-pharmacologic options for those fighting drug addiction, notably chiropractic care. When paired with the U.S. Surgeon General’s declaration of war on addiction,8 the government’s designation of “Prescription Opioid and Heroin Epidemic Awareness Week,” 9 and the commitment from 40 prescriber groups to ensure that 540,000 health care providers would complete training on appropriate opioid prescribing within two years,10 these “solutions” appear woefully inadequate to address the challenges of those who need effective, drug- free pain management.
This follow-up discussion to “Chiropractic: A Safer Strategy than Opioids” (June 2016), examines the positive steps as well as the shortcomings of initiatives undertaken from July 2016 – March 2017 to address the opioid crisis. It also assesses the current landscape of opportunities to offer patients, doctors and payers meaningful programs to effectively address acute, subacute and chronic neck, low back and neuro-musculoskeletal pain without the use of painkillers.
The chiropractic profession contends this should be a top priority, and it appears that a growing number of stakeholders are in agreement. In fact, the world’s second-largest pharmaceutical company has agreed to disclose in its marketing material that opioid painkillers might carry a serious risk of addiction, and promised not to promote prescription opioids for unapproved uses, such as long-term back pain.11
Based upon the evidence articulated in this document, it becomes clear that chiropractic care is a key component of “America’s Opioid Exit Strategy” on several levels:
- Perform first-line assessment and care for neck, back and neuro-musculoskeletal pain to avoid opiate prescribing from the first onset of pain.
- Provide care throughout treatment to mitigate the introduction of drugs.
- Offer an effective approach to acute, subacute and chronic pain management that helps addicts achieve a wellness focused, pain-free lifestyle as they reduce their utilization of opioids.
It’s also a compelling opportunity for our health system, commercial and government payers, employers — and most importantly patients — to resolve the issues surrounding pain at lower costs, with improved outcomes and without drugs or surgery.
Further complicating the situation: escalating prices of the opioid OD drug naloxone may threaten efforts to reduce opioid-related deaths across America, warn teams at Yale University and the Mayo Clinic.13
Naloxone is a drug given to people who overdose on prescription opioids and heroin. If administered in time, it can reverse the toxic and potentially deadly effects of “opioid intoxication.”
The research team called attention to skyrocketing prices for the lifesaving antidote, noting:
- Hospira (a Pfizer Inc. company) charges $142 for a 10-pack of naloxone — up 129 percent since 2012.
- Amphastar’s 1 milligram version of naloxone is used off-label as a nasal spray. It’s priced around $40 — a 95 percent increase since September 2014.
- Newer,easier-to-use formulations are even more expensive — a two-dose package of Evzio (naloxone) costs $4,500, an increase of more than 500 percent over two years.“The challenge is as the
price goes up for naloxone, it becomes less accessible for patients,” said Ravi Gupta, the study’s lead author.
Table of Contents
Government & Regulators Restrict Access To Opioids
In the wake of this firestorm surrounding opioid abuse, and following the dissemination of prescribing guidelines introduced by the CDC, it becomes evident that certain market forces are influencing the battle against opioid addiction and the availability of drugs.
Among the most egregious stakeholders are those in the pharmaceutical sector.There are numerous instances which document their role attempting to thwart many legislative initiatives throughout the country to combat drug abuse.They impose exorbitant costs for life-saving antidotes, and aggressively develop and market the use of more drugs to fight opioid-induced side effects such as constipation. It becomes apparent that many of their answers to opioid addiction are simply more pills.14
The opioid market is worth nearly $10 billion in annual sales, and has expanded to include an unlimited universe of medications aimed at treating secondary effects rather than controlling pain.15 Given the financial incentives to produce, sell and distribute drugs, it’s no wonder that pharmaceutical companies (pharmcos) have a material interest in promoting drug utilization.
This set of behaviors has drawn extensive criticism.
“The root cause of our opiate epidemic has been the over-prescribing of prescription pain medications. Physicians get little to no training related to addiction in general, but particularly around opiate prescriptions. Over the past year, however, you hear more and more physicians admitting ‘we are part of the problem and can be part of the solution’.”16
—- Michael Botticelli, former White House drug policy director, commonly called the nation’s drug czar.
While physicians have been responding to calls for more responsible prescribing, the drug industry has historically been accused of providing physicians with misleading information regarding the addictive qualities of certain drugs.Appropriate education of prescribers is a key component of necessary change.
For example, when semisynthetic opioids like oxycodone and hydrocodone — found in Percocet and Vicodin respectively — were first approved in the mid–20th century, they were recommended only for managing pain during terminal illnesses such as cancer, or for acute short-term pain, like recovery from surgery, to ensure patients wouldn’t get addicted. But in the 1990s, doctors came under increasing pressure to use opioids to treat the millions of Americans suffering from chronic non-malignant conditions, like back pain and osteoarthritis.
A physician pain specialist helped lead the campaign, claiming prescription opioids were a “gift from nature,” with assurances to his fellow doctors — based on a 1986 study of only 38 patients — that fewer than one percent of long-term users became addicted.17
Today, drug makers may be getting their ‘wings clipped’ with the introduction of new government directives slashing production of popular prescription painkillers. In 2016, the U.S. Drug Enforcement Administration (DEA) finalized a previous order on 2017 production quotas for a variety of Schedule I and II drugs, including addictive narcotics like oxycodone, hydromorphone, codeine and fentanyl. The agency has the authority to set limits on manufacturing under the Controlled Substances Act. The DEA said it is reducing “the amount of almost every Schedule II opiate and opioid medication” by at least 25 percent.18 Some, like hydrocodone, commonly known by brand names like Vicodin or Lortab, will be cut by one-third.
Despite these setbacks, the drug industry continues to launch strong initiatives that fight state- mandated opioid limits. Amid the crisis and regardless of the pressures urging a shift away from opioid use, the makers of prescription painkillers recently adopted a 50-state strategy that includes hundreds of lobbyists and millions in campaign contributions to help kill or weaken measures aimed at stemming the tide of prescription opioids.19
While the drug makers vow they’re combating the addiction problem,The Associated Press
and the Center for Public Integrity found that these manufacturers often employ a statehouse playbook of delay and defend tactics.This includes funding advocacy groups that use the veneer of independence to fight limits on the drugs, such as OxyContin, Vicodin and Fentanyl, a potent, synthetic opioid pain medication with a rapid onset and short duration of action that is estimated to be between 50 and 100 times as potent as morphine.20
In its national update released Dec. 16, 2016 in the Morbidity and Mortality Weekly Report, the CDC reported that more than 300,000 Americans have lost their lives to an opioid overdose since 2000.
As enforcement restricts the availability of prescription opioids, people addicted
to painkillers — such as oxycodone (OxyContin) and morphine — have increasingly turned to — street drugs like heroin.21
These independent sources also found that the drug makers and allied advocacy groups employed an annual average of 1,350 lobbyists in legislative hubs from 2006 through 2015, when opioids’ addictive nature came under increasing scrutiny.
“The opioid lobby has been doing everything it can to preserve the status quo of aggressive prescribing.They are reaping enormous profits from aggressive prescribing.”22
Andrew Kolodny, MD, founder, Physicians for Responsible Opioid Prescribing
Undaunted by these interferences, and buoyed by a thirst for profits, pharmcos are now fueling other creative solutions to drive even greater revenues from the sale and distribution of drugs.
It now appears that pharmcos are directing their activities toward medicines known as abuse-deterrent formulations: opioids with physical and/or chemical barriers have built-in properties that make the pills difficult to crush,chew or dissolve.This aims to deter abuse through intranasal and intravenous routes of administration.These drugs ultimately are more lucrative, since they’re protected by patent and do not yet have generic competitors.They cost insurers more than generic opioids without the tamper-resistant technology.23
Skeptics warn that they carry the same risks of addiction as other opioid versions, and the U.S. FDA noted that they don’t prevent the most common form of abuse — swallowing pills whole.
“This is a way that the pharmaceutical industry can evade responsibility, get new patents and continue to pump pills into the system,” said Dr. Anna Lembke, Chief of Addiction Medicine at the Stanford University School of Medicine.24
Drug makers have discovered yet another way to profit from addicts taking high doses of prescription opioid painkillers – the new billion-dollar drug to treat opioid-induced constipation (OIC) rather than controlling pain.
Studies show that constipation afflicts 40-90 percent of opioid patients.Traditionally,doctors advised people to cut down the dosage of their pain meds, take them less often or try non-drug interventions. By promoting OIC as a condition in need of more targeted treatment, the drug industry is creating incentives to maintain painkillers at full strength and add another pill instead.25
Collectively, the subsets of new pharmaceutical submarkets to treat opioid addiction, overdoses, and side effects such as OIC are estimated to be worth at least $1 billion a year in sales.These economics, some experts say, work against efforts to end the epidemic.26
While there is continued pressure to limit the number and scope of opiates for patients, new government statistics reveal that drug overdose deaths continue to surge in the United States, now exceeding the number of deaths caused by motor vehicle accidents.27 Although it is reported that the number of opioid prescriptions has fallen across the U.S. over the past three years, with intermittent data on this decline in states such as West Virginia and Ohio, they still kill more Americans each year than any other drug.
Just over 33,000 (63 percent) of the more than 52,000 fatalities reported in 2015 are linked to the illicit use of prescription painkillers.28 States including Massachusetts, and most recently Virginia, have declared public health emergencies as the number of deaths has escalated.29
Regardless of whether these issues are viewed from the perspective of patients, clinician prescribers, or government regulators, the status quo is clearly not acceptable.
Responsible Prescribing
“My new patient didn’t mention his back pain until the very end of the visit.As he was rising to leave, he asked casually if I could refill his Percocet. I told him I am not a pain or a back specialist and that I generally prescribe muscle relaxants or anti-inflammatory medications for back pain — not opioids, which are addictive and do not really treat the underlying problem.
The patient persisted. He said his prior internist always prescribed it, and the medication also helped his mood. He promised he had its use under control and did not feel he needed to take more and more to achieve the same effect.
I didn’t relent. I offered to refer him to a back specialist instead. It was an uncomfortable end to an otherwise positive visit.
Unfortunately, we doctors are enablers.Too many of us fill those prescriptions for chronic pain. And when we don’t, too many of our patients leave us for other doctors who will. Or worse, they turn to buying heroin on the street.”30
Marc Siegel, MD, FOX NEWS
Clinical prescribers of pain medications are beginning to recognize their responsibilities for increased prescribing vigilance, and are expected to become important advocates for drug-free pain care. More than half of doctors across America are curtailing opioid prescriptions, and nearly 1 in 10 have stopped prescribing the drugs, according to a new nationwide online survey. More than one-third of the respondents said the reduction in prescribing has hurt patients with chronic pain.
The survey, conducted for The Boston Globe by the SERMO physicians social network, offers fresh evidence of the changes in prescribing practices in response to the opioid crisis that has killed thousands in New England and elsewhere around the country.The deaths awakened fears of addiction and accidental overdose, and led to state and federal regulations aimed at reining in excessive prescribing.
Doctors face myriad pressures as they struggle to treat addiction and chronic pain, two complex conditions in which most physicians receive little training.Those responding to the survey gave two main reasons for cutting back: the risks and hassles involved in prescribing opioids, and a better understanding of the drugs’ hazards.31
In Wisconsin, the Medical Society says the state’s effort to fight the opioid epidemic is showing results.A new report found about eight million fewer opioids were dispensed between July and September 2016 compared to the same time during the previous year.The Medical Society says it’s doing more to help physicians monitor patients’ use of opioids by supporting the release of an enhanced prescription drug monitoring program – or PDMP. Starting in April 2017, doctors will have to access the program while pharmacists will only have 24 hours to enter information instead of seven days.This gives doctors an update in case patients are going from doctor to doctor for more prescriptions.32
Prescription drug monitoring programs (PDMPs), launched in 2013, are state-run electronic databases used to track the prescribing and dispensing of controlled prescription drugs to patients.They are designed to monitor this information for suspected abuse or diversion (i.e., channeling drugs into illegal use), and can give a prescriber or pharmacist critical information regarding a patient’s controlled substance prescription history.This information can help prescribers and pharmacists identify patients at high-risk who would benefit from early interventions.
PDMPs continue to be among the most promising state-level interventions to improve opioid prescribing, inform clinical practice and protect patients at risk.33
Hospital Admissions Due To Heroin, Painkillers Rose 64% 2005-2014
Researchers found misuse of prescription painkillers and street opioids climbed nationwide, related hospital stays jumped from 137 per 100,000 people to 225 per 100,000 in that decade.
States where overdoses required at least 70 percent more hospital beds between 2009 and 2014 were North Carolina, Oregon, South Dakota and Washington.
In 2014, the District of Columbia, Maryland, Massachusetts, New York, Rhode Island and West Virginia each reported rates above 300 per 100,000 people — far above the national average.34
Health Plans Report Limited Prescribing Is Paying Off
According to IMS Health, a global health information and technology firm, the rate of opioid prescribing in the U.S. has dropped since its peak in 2012.The drop is the first that has been reported since the early 1990s, when OxyContin first hit the market and pain became “the fifth vital sign” doctors were encouraged to more aggressively treat.35
However, continued pressure on physician prescribing patterns and opportunities for therapies other than opioids may be paying off. Prescriptions for powerful painkillers dropped significantly among patients covered by Massachusetts’ largest insurer after measures were introduced to reduce opioid use.36 The Blue Cross Blue Shield of Massachusetts program serves as an example of a private health insurer collaborating on a public health goal.
In 2012, the insurer — the state’s largest, with 2.8 million members — instituted a program intended to induce doctors and patients to weigh the risks of opioids and consider alternatives.As part of that initiative, first-time opioid prescriptions are limited to 15 days, with a refill allowed for 15 more days. Blue Cross must approve in advance any prescription for longer than a month or for any long-acting opioid such as OxyContin. Pharmacy mail orders for opioids are prohibited.
Doctors and others who prescribe must assess the patient’s risk of abusing drugs and develop a treatment plan that considers options other than opioids. And patients with chronic pain are referred to case managers who advise on therapies other than opioids.
By the end of 2015, the average monthly prescribing rate for opioids decreased almost 15 percent, from 34 per 1,000 members to 29. About 21 million fewer opioid doses were dispensed during the three years covered in the study.37
In another example, Highmark (Pennsylvania) shared data in December 2016 showing that the number of prescriptions for opioids it reimbursed in each of the past three months was lower than in any of the prior nine months. One leading health plan in the state reported that 16 percent of its insured population received at least one opioid prescription in 2016, down from 20 percent in 2015.38 UPMC Health Plan indicated it is using “an algorithm to identify patients who may be at risk for opioid addiction,” and training doctors to use other pain management tools.
Mounting Evidence & Support For Non-Pharmacologic Care For Acute, Subacute & Chronic Back, Neck & Neuro-Musculoskeletal Pain
The earlier sections of this white paper have focused on the continuing and growing problem of opioid use, abuse and addiction. It is essential that this information is understood and appreciated as it clearly calls for a wholesale change in the approach American health care providers and patients bring to the care and management of pain.
No matter what is done to address the use, abuse and addiction associated with opioids it is a fact of life that opioid containing products will continue to be required by individuals suffering severe, intractable and unrelenting pain.This issue is not about the cessation of all opioid use, rather it is about not turning to opioids before they are required, and not until all less onerous approaches to pain management have been exhausted.

We began this discussion with three questions in mind:
- Without the use of drugs, how will they cope with pain?
- How can they get referrals and access to drug-free care that will be effective for both acute, subacute and chronic pain?
- How can they ensure that their health care plans and insurance will cover the cost of non- pharmacologic care?
According to new guidelines developed by the American College of Physicians,39 conservative non-drug treatments should be favored over drugs for most back pain. The guidelines are an update that include a review of more than 150 recent studies and conclude that,“For acute and subacute pain, the guidelines recommend non-drug therapies first, such as applying heat, massage, acupuncture, or spinal manipulation, which is often done by a chiropractor.”
The Wall Street Journal
As we have previously noted the CDC, FDA and IOM have all called for the early use of non- pharmacologic approaches to pain and pain management. Unfortunately, beyond asserting the need to move in this direction, little, if any, guidance has been offered to providers, patients and payors on how to accomplish this important transition.
It is a fact that a chasm exists between the worlds of pharmacologic based management of pain, and the non-pharmacologic based management of pain. Medical physicians are not going to suddenly attain knowledge and understanding of practices, procedures and management options that they have never been trained in or exposed to. Similarly, the non-pharmacologic providers addressing pain management do not encounter or understand the barriers that prevent prescribers from directing patients toward non-pharma approaches.These two spheres of healthcare are distinct and separate, and demonstrate little, if any, knowledge about the other.
The first step is to provide resources to prescribers that will detail the indications, effectiveness, efficiency and safety of non-pharmacologic approaches. In particular, the chiropractic profession, through its 70,000 practitioners in the United States, represents a significant and proven non- pharmacologic approach for reducing the need for opioids, opioid-related products and non- opioid pain medications.
Chiropractic, like other complementary health care approaches, suffers from a lack of awareness about its high level of education, credentialing and regulation. In addition, a substantial awareness gap exists among frontline providers in terms of referring patients to chiropractors as part of patient care.
The chiropractic profession and the health care consumer are equally supported by a robust oversight infrastructure.This infrastructure ranges from institutional and programmatic accreditation of chiropractic education by agencies recognized by the U.S. Department of Education to standardize national credentialing examinations and licensure by state agencies and ongoing professional development as a requirement for continued practice in many states.
Typically, after earning a Bachelor of Science, chiropractors follow a four-year curriculum to earn a Doctor of Chiropractic (DC) as a prerequisite to earning the right to independent practice. Chiropractic, medical, osteopathic, dental, optometric and naturopathic education share a similar foundation in the basic sciences, followed by discipline-specific content that focuses on the unique contribution of each provider type. For example, a medical student pursues the study of pharmacology and surgery, while a chiropractic student studies the intricacies of manual approaches to health care and the acquisition of the skills needed to perform spinal adjusting or manipulation.
Chiropractors also pursue specialization in specific areas, such as radiology, through structured residency programs, similar to other disciplines. DCs also pursue focus areas related to various methods of spinal adjusting and related patient management.
For over a century, DCs have studied the relationship between structure, primarily the spine, and function, primarily of the nervous system, and how this interrelationship impacts health and well- being. Due to this emphasis on the spine, chiropractors have become associated with spinal and skeletal pain syndromes, and bring their non-surgical, non-drug rationale to the management of these problems.
DCs are the quintessential example of non-pharmacologic providers of health care with particular expertise in neuro-musculoskeletal conditions.
A Look At The Evidence
While the United States is attempting to deal with its opioid epidemic, our nation is making only limited headway in providing non-pharmacologic approaches to patients with pain.
Over 100 million Americans suffer with chronic pain,40 and an estimated 75 to 85 percent of all Americans will experience some form of back pain during their lifetime. However, 50 percent of
all patients who suffer from an episode of low back pain will have a recurrent episode within one year.41 Surgery has a very limited role in the management of spinal pain, and is only considered appropriate in a handful of cases per hundred patients. Likewise, opioids have very limited utility in the spinal pain environment with the recommended use of these drugs being limited to three days.
Of special relevance, this data relates to the most commonly-report
Post Disclaimer
Professional Scope of Practice *
The information on this blog site is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice.*
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933



Comments are closed.